|
Vocapedia >
Health > Viruses
>
Retro-viruses >
Syndrom > AIDS

Title : When Martin was told he had
AIDS,
his family couldn't believe it. After all, he is 64
Creators : London Lighthouse [Publisher]
Current Repository :
Louise M. Darling Biomedical Library.
History & Special
Collections
Dimensions : 60 x 43 cm. (24 x 17 in.)
Publication Location : London
Date : [between 1988 and 2000]
Note : Black and white photograph
of three smiling people
sitting on a blanket
in the grass:
a middle-aged man and woman, and a young man.
Poster suggests that anyone can be infected with AIDS,
not just young gay men,
and describes London Lighthouse
as a resource for older people who are
HIV-positive.
: Poster held by Louise M. Darling Biomedical Library.
History & Special
Collections,
Collection no. 306, item UK016.
Date on back of poster, 1996,
reflects when the vendor received the copy
later
acquired by the UCLA Library.
http://digital.library.ucla.edu/aidsposters/librarian?ITEMID=UK016_a
http://digital.library.ucla.edu/aidsposters/

Dorika Gabriel
carries her 30-year-old son Joseph to shade,
Tanzania, 1997.
Photograph:
Gideon Mendel
Corbis
Gideon Mendel's best photograph:
a mother carries her HIV-infected son
G
Thu 29 Nov 2018 06.00 GMT
Last modified on Thu 29 Nov 2018 09.26 GMT
https://www.theguardian.com/artanddesign/2018/nov/29/
gideon-mendel-best-photograph-mother-carries-hiv-infected-son

March or April 2020.
1997
Caption and URL in a next edition.
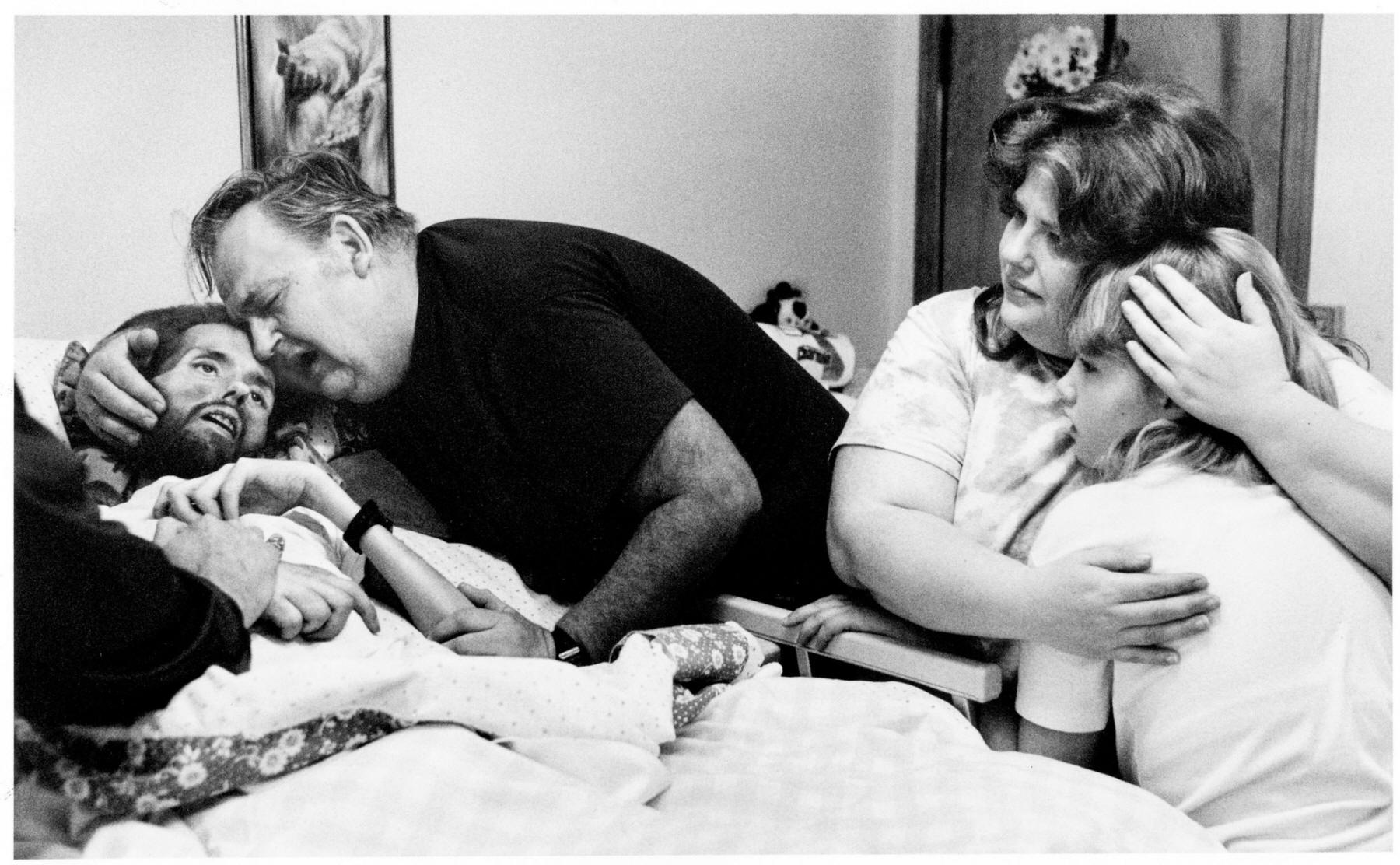
[
David Kirby
on his deathbed, Ohio,
1990. ]
Therese Frare’s “Final Moments” (1990).
Photograph:
Therese Frare
Bruce Silverstein Photography
What Can We Learn From the Art of Pandemics Past?
From the playground game ring-around-the-rosy
to the short stories of Edgar Allan Poe,
the scars of illnesses throughout history are still visible
today.
NYT
April 8, 2020
https://www.nytimes.com/2020/04/08/
t-magazine/art-coronavirus.html
What is HIV
and AIDS? UK
https://www.bbc.co.uk/worldservice/sci_tech/features/health/
sexualhealth/aids/what.shtml
NPR podcasts > 2025
NPR podcasts > before 2025
Acquired Immune Deficiency Syndrome AIDS FR / UK / USA
AIDS pandemic
AIDS
(acquired immune deficiency syndrome)
is the final stage of HIV disease,
which causes severe damage to the immune system.
http://health.nytimes.com/health/guides/disease/
aids/overview.html - broken URL
The AIDS epidemic was
(and still is, in some communities)
a catastrophe no one predicted.
Throughout the 1980sin New York City,
there was little government support
for those who contracted the virus
— a symptom of the era’s discrimination against minorities,
intravenous drug users and gay people.
Ignorance about or shame
associated with what was called the ‘‘gay plague’’
was prevalent.
Given the high rate with which gay men died,
certain fields of enormous creativity and change
— from art to fashion to literature —
were devastated, never to recover completely.
(Among women,
African-American women were, and still are,
disproportionately affected.)
https://www.nytimes.com/interactive/2018/04/17/
t-magazine/aids-epidemic-deaths-new-york.html - 2018
https://en.wikipedia.org/wiki/HIV/
AIDS
2026
https://www.nytimes.com/2026/05/08/
world/africa/festus-mogae-dead.html
https://www.nytimes.com/2026/04/25/
health/pepfar-hiv-aids-zambia.html
https://www.theguardian.com/music/2026/feb/04/
gay-porn-soundtrack-composers-lost-to-aids-crisis-80s
2025
https://www.npr.org/2025/09/12/
nx-s1-5539546/can-the-global-hiv-aids-fight-recover-
from-trumps-cuts
https://www.nytimes.com/2025/07/14/
health/south-africa-aids-hiv-trump-funding-cuts.html
2024
https://www.npr.org/sections/shots-health-news/2024/06/15/
nx-s1-4990795/hiv-aids-aging-health-risks-funding
https://www.npr.org/2024/02/21/
1233022530/hydeia-broadbent-hiv-aids-activist-
dies-age-39
2023
https://www.npr.org/2023/05/27/
1178084648/keith-haring-radiant-baby-the-broad
https://www.npr.org/sections/goatsandsoda/2023/01/26/
1150851465/why-inventing-a-vaccine-for-aids-
is-tougher-than-for-covid
2021
https://www.npr.org/sections/goatsandsoda/2021/07/29/
1022298151/ambitious-plan-to-stem-hiv-aids-epidemic-
meets-none-of-its-goals
https://www.nytimes.com/2021/06/04/
nyregion/ganga-stone-dead.html
https://www.nytimes.com/2021/05/20/
books/review/let-the-record-show-sarah-schulman.html
https://www.theguardian.com/stage/2021/apr/05/
aids-plays-normal-heart-angels-in-america-enduring-power-anger
https://www.npr.org/2021/02/17/
968365774/its-a-sin-
series-set-during-aids-epidemic-resonates-during-covid-19
2020
https://www.theguardian.com/society/2020/dec/01/
through-positive-eyes-living-with-hiv-and-aids-a-photo-essay
https://www.npr.org/sections/goatsandsoda/2020/11/19/
936627318/long-lasting-anti-aids-meds-eliminate-
psychic-toll-of-daily-pill
https://www.nytimes.com/2020/10/27/
us/joyce-wallace-dies.html
https://www.npr.org/2020/08/03/
898581035/they-know-what-a-pandemic-is-
hiv-survivors-see-similarities-to-aids-epidemic
https://www.nytimes.com/2020/06/18/
us/coronavirus-aids-epidemic-lessons.html
https://www.npr.org/2020/05/29/
864935788/remembering-pioneering-aids-activist-larry-kramer
https://www.nytimes.com/2020/05/27/
theater/larry-kramer-playwright-appraisal.html
https://www.nytimes.com/2020/05/27/
health/larry-kramer-anthony-fauci.html
https://www.theguardian.com/stage/gallery/2020/may/27/
larry-kramer-life-in-pictures
https://www.theguardian.com/us-news/2020/may/27/
larry-kramer-death-playwright-author-hiv-aids-activist
https://www.nytimes.com/2020/05/20/
arts/dance/bill-t-jones-deep-blue-sea.html
https://www.nytimes.com/2020/05/16/
world/americas/virus-brazil-deaths.html
https://www.theguardian.com/stage/gallery/2017/apr/28/
angels-in-america-national-theatre-in-pictures
https://www.nytimes.com/interactive/2020/04/13/
t-magazine/act-up-aids.html
https://www.nytimes.com/2020/04/08/
t-magazine/art-coronavirus.html
https://www.nytimes.com/2020/03/28/
nyregion/coronavirus-larry-kramer-aids.html
https://www.npr.org/2020/03/17/
813631154/later-takes-us-to-1990s-provincetown-
as-hope-for-aids-treatment-rises
https://www.wbur.org/hereandnow/2020/03/09/
pandemics-coronavirus-aids-flu
2019
- Ce qui a rendu possible l'épidémie du sida -
Video - Mediapart - 20 October 2019 - FR
https://www.youtube.com/
watch?v=vNuy3tCOJNc
https://www.npr.org/sections/health-shots/2019/06/26/
736060834/1st-aids-ward-5b-fought-to-give-patients-compassionate-care-dignified-deaths
https://www.npr.org/sections/health-shots/2019/05/30/
727731380/old-fight-new-front-aids-activists-want-lower-drug-prices-now
https://www.theguardian.com/lifeandstyle/2019/apr/20/
i-tried-to-save-my-brother-whose-early-death-made-me-the-person-i-am
https://www.npr.org/sections/health-shots/2019/02/09/
689924838/how-to-demand-a-medical-breakthrough-lessons-from-the-aids-fight
2018
https://www.nytimes.com/2018/09/07/
magazine/the-rage-and-tenderness-of-david-wojnarowiczs-art.html
https://www.npr.org/2018/07/22/
631254992/4-years-after-mh17-downing-advocates-urge-continued-attention-to-aids-crisis
https://www.nytimes.com/2018/07/12/
arts/design/david-wojnarowicz-review-whitney-museum.html
https://www.npr.org/2018/07/04/
625355423/a-stage-revival-and-50-years-of-survival-for-the-boys-in-the-band
https://www.nytimes.com/2018/07/03/
nyregion/hart-island-aids-new-york.html
https://www.nytimes.com/2018/06/26/
opinion/gay-men-sex-condoms.html
https://www.nytimes.com/2018/06/25/
books/review/rebecca-makkai-great-believers.html
https://www.nytimes.com/interactive/2018/04/17/
t-magazine/aids-epidemic-deaths-new-york.html
https://www.nytimes.com/2018/01/16/
obituaries/mathilde-krim-mobilizing-force-in-an-aids-crusade-dies-at-91.html
2017
https://www.npr.org/sections/thesalt/2017/11/24/
566387319/how-one-pop-up-restaurant-is-fighting-stigma-
against-hiv-aids
https://www.nytimes.com/2017/10/11/
theater/michael-friedman-aids-death-theater.html
http://www.npr.org/2017/08/04/
541658697/pharma-bro-martin-shkreli-convicted-of-securities-fraud
https://www.nytimes.com/2017/06/13/
well/family/
losing-a-father-and-husband-to-aids-and-finding-him-again.html
https://www.nytimes.com/2017/02/09/
opinion/bill-frist-the-case-for-keeping-americas-aids-relief-plan.html
2016
https://www.npr.org/sections/health-shots/2016/10/26/
498876985/mystery-solved-how-hiv-came-to-the-u-s
https://www.nytimes.com/2016/09/18/
arts/dance/honoring-dance-innovators-lost-to-aids.html
https://www.theguardian.com/global-development/2016/jul/31/
aids-epidemic-getting-worse-drug-resistance-cost
https://www.theguardian.com/global-development/2016/jul/31/
aids-could-spiral-out-control-africa-again-experts-warn
http://www.nytimes.com/2016/07/29/
arts/design/art-of-the-aids-years-addressing-history-absorbing-fear.html
http://www.nytimes.com/2016/06/13/
opinion/the-world-could-end-aids-if-it-tried.html
http://www.theguardian.com/society/commentisfree/2016/apr/20/
a-generation-of-artists-were-wiped-out-by-aids-
and-we-barely-talk-about-it-robert-mapplethorpe
http://www.nytimes.com/2016/03/06/
health/dr-myron-g-schultz-who-helped-identify-aids-crisis-dies-at-81.html
http://www.npr.org/sections/health-shots/2016/02/25/
467968807/the-aids-crisis-hasnt-ended-in-the-black-and-latino-communities
2015
http://www.npr.org/2015/12/04/
458211617/for-a-schoolboy-with-aids-
a-principal-opened-doors-by-opening-his-arms
http://www.nytimes.com/2015/12/02/
opinion/an-opening-in-the-war-against-aids.html
http://www.nytimes.com/2015/12/02/
health/us-still-in-danger-of-losing-war-on-aids-cdc-director-says.html
http://www.theguardian.com/commentisfree/2015/sep/04/
hiv-positive-leak-patients-stigma
http://www.nytimes.com/2015/02/19/
health/new-approach-to-blocking-hiv-raises-talk-of-an-aids-vaccine.html
2014
http://www.nytimes.com/2014/05/15/
health/advocating-pill-us-signals-shift-to-prevent-aids.html
http://www.nytimes.com/2014/05/15/
opinion/blow-the-aids-shaming-of-magic-johnson.html
http://www.nytimes.com/2014/03/25/
theater/mothers-and-sons-an-aids-tale-starring-tyne-daly.html
2013
http://www.nytimes.com/2013/09/15/
health/stephen-crohn-who-furthered-aids-study-dies-at-66.html
2012
http://www.nytimes.com/2012/07/28/
opinion/imagine-a-world-without-aids.html
http://www.nytimes.com/2012/07/28/
opinion/the-long-uphill-battle-against-aids.html
2011
http://www.nytimes.com/2011/12/01/
opinion/a-decade-of-progress-on-aids.html
https://www.npr.org/sections/pictureshow/2011/12/01/
142998189/the-photo-that-changed-the-face-of-aids
http://www.reuters.com/article/2011/06/03/
us-aids-policy-idUSTRE7520RQ20110603
http://www.reuters.com/article/2011/06/01/
us-aids-idUSTRE75030I20110601
http://www.nytimes.com/2010/05/14/
opinion/14fri2.html
http://www.nytimes.com/2010/05/10/world/africa/
10aids.html
http://www.guardian.co.uk/global/2008/jul/29/aids
http://www.theguardian.com/world/2006/dec/01/aids
http://www.nytimes.com/2005/05/01/nyregion/
01novick.html
https://www.nytimes.com/2003/11/11/
science/what-did-we-learn-from-aids.html
https://www.nytimes.com/1993/12/10/
world/british-paper-and-science-journal-clash-on-aids.html
https://www.nytimes.com/1991/01/25/
us/us-reports-aids-deaths-now-exceed-100000.html
https://www.nytimes.com/1989/06/29/
opinion/why-make-aids-worse-than-it-is.html
https://www.nytimes.com/1987/12/30/
opinion/aids-the-end-of-the-beginning.html
https://www.nytimes.com/1987/11/08/
books/plenty-of-blame-to-go-around.html
https://www.nytimes.com/1987/02/13/
nyregion/funerals-for-aids-victims-searching-for-sensitivity.html
1986
https://www.nytimes.com/1986/12/17/
us/aids-immunization-tested-on-humans.html
https://www.nytimes.com/1986/12/13/
us/aids-may-spread-outside-bloodstream.html
https://archive.nytimes.com/www.nytimes.com/books/
00/07/16/specials/buckley-aids.html - March 18, 1986
https://archive.nytimes.com/www.nytimes.com/library/
national/science/aids/101585sci-aids.html
1985
https://www.nytimes.com/1985/08/30/
nyregion/fear-of-aids-grows-among-heterosexuals.html
https://www.nytimes.com/1985/08/09/
opinion/how-to-fight-aids.html
1984
https://www.nytimes.com/1984/04/22/
us/federal-official-says-he-believes-cause-of-aids-has-been-found.html
1983
https://www.nytimes.com/1983/11/29/
science/aids-now-seen-as-a-worldwide-health-problem.html
https://www.nytimes.com/1983/02/06/
magazine/aids-a-new-disease-s-deadly-odyssey.html
AIDS > patient zero USA
http://www.npr.org/sections/health-shots/2016/10/26/
498876985/mystery-solved-how-hiv-came-to-the-u-s
USA > the AIDS Crisis hasn't ended
In the Black And Latino communities
USA 2016
http://www.npr.org/sections/health-shots/2016/02/25/
467968807/the-aids-crisis-hasnt-ended-in-the-black-and-latino-communities
AIDS > monkeys
USA
http://www.nytimes.com/2014/03/05/
health/injections-provide-durable-protection-against-aids-in-monkeys-studies-find.html
onset of AIDS Aids
fight the spread of AIDS
USA
http://www.nytimes.com/2009/10/27/
health/27hiv.html
the scourge of AIDS
USA
http://theater.nytimes.com/2010/05/11/
theater/reviews/11letters.html
Sharing Burdens of Living With AIDS
USA
http://www.nytimes.com/2011/09/27/
health/27mozambique.html
Ward 5B,
the first inpatient special care hospital unit
for treating people with AIDS - 1983
USA
In the early years of the AIDS epidemic,
when the disease didn't have a name
and no one knew what caused it
or how it was spread,
(...) Dr. Paul Volberding
and nurse Cliff Morrison,
were taking care of people
who were infected,
very sick and dying.
Now they're featured
in a new documentary
titled "5B" about Ward 5B,
the first inpatient
special care hospital unit
for treating people with AIDS.
The unit opened
in San Francisco General Hospital
in 1983,
the year that HIV was identified
as the cause of AIDS.
It became a model
for AIDS treatment in the U.S.,
as well as other countries.
https://www.npr.org/sections/health-shots/2019/06/26/
736060834/1st-aids-ward-5b-fought-to-give-patients-compassionate-care-dignified-deaths
https://www.npr.org/sections/health-shots/2019/06/26/
736060834/1st-aids-ward-5b-fought-to-give-patients-compassionate-care-dignified-deaths
the war on Aids / fighting Aids
USA
http://www.nytimes.com/2010/05/15/
opinion/l15aids.html
http://www.nytimes.com/2010/05/14/
opinion/14fri2.html
AIDS symbol UK
http://www.guardian.co.uk/world/2010/nov/23/world-
aids-day-2010-boseley
Aids orphans UK
https://www.theguardian.com/society/2006/aug/16/
health.aids
Worldwide Aids epidemic slowing, says UN
UK
July 29, 2008
https://www.theguardian.com/global/2008/jul/29/
aids
17th International AIDS Conference
USA
http://www.nytimes.com/2008/08/04/
health/04aids.html
World Aids Day
1 December UK
https://www.worldaidsday.org.au/
about
http://www.guardian.co.uk/global-development/2011/nov/30/
world-aids-day-hiv-live-chat
http://www.guardian.co.uk/world/interactive/2009/nov/21/
aids-kenya-gideon-mendel
http://www.guardian.co.uk/world/gallery/2009/dec/01/
outlook-brazil
full-blown Aids UK
http://www.guardian.co.uk/global/2008/jul/29/
aids
full-blown AIDS USA
https://www.nytimes.com/2017/06/13/
well/
family/losing-a-father-and-husband-to-aids-and-finding-him-again.html
AIDS
patient USA
http://www.nytimes.com/2008/11/14/
health/14hiv.html
stigma USA
http://www.nytimes.com/2010/07/12/
health/policy/12aids.html
AIDS > Africa USA
https://www.nytimes.com/2015/12/12/
opinion/why-are-so-many-black-women-dying-of-aids.html
AIDS > Cambodia UK
https://www.theguardian.com/world/2004/oct/17/
aids.cambodia
AIDS > India UK /
USA
https://www.nytimes.com/2012/11/25/
world/asia/indian-prostitutes-new-autonomy-imperils-aids-fight.html
http://www.independent.co.uk/life-style/love-sex/
sex-industry/indias-sex-trade-exposed-1036578.html
AIDS > South Africa
USA
http://www.nytimes.com/2008/11/26/world/africa/
26aids.html
http://graphics8.nytimes.com/packages/pdf/world/20081125
_AIDS_Document.pdf
AIDS > Uganda USA
http://www.nytimes.com/2010/05/10/world/africa/
10aids.html
AIDS > circumcision USA
http://www.npr.org/blogs/health/2014/05/07/
310465206/snip-decision-africas-campaign-to-circumcise-its-men
https://www.nytimes.com/2009/08/24/
health/policy/24circumcision.html
AIDS activist USA
https://www.nytimes.com/2025/07/14/
health/south-africa-aids-hiv-trump-funding-cuts.html
https://www.npr.org/2024/02/21/
1233022530/hydeia-broadbent-hiv-aids-activist-dies-age-39
https://www.nytimes.com/2010/12/01/us/
politics/01aids.html
AIDS activist > Jeff Getty
USA
https://www.nytimes.com/2006/10/16/
health/16getty.html
UNAIDS > United Nations program on AIDS/HIV
https://www.unaids.org/en
AIDS pandemic UK / USA
http://www.guardian.co.uk/society/2010/oct/08/
hiv-infections-rise-20-years
https://www.theguardian.com/society/2006/may/31/health.aids
http://www.nytimes.com/2005/06/03/health/03aids.html
http://www.nytimes.com/2005/06/03/international/africa/03mozambique.html
http://www.nytimes.com/2005/05/11/international/africa/11malawi.html
http://www.nytimes.com/2005/02/15/health/15aids.html
http://www.theguardian.com/politics/2005/feb/15/uk.conservatives
https://www.theguardian.com/science/2004/dec/10/southafrica.internationalaidanddevelopment
https://www.theguardian.com/society/2004/nov/23/internationalaidanddevelopment.aids
https://www.theguardian.com/world/2004/feb/16/aids
https://www.theguardian.com/society/2004/feb/15/aids.medicineandhealth
http://www.guardian.co.uk/microsite/mariestopes/hivaids/
https://www.theguardian.com/world/2003/oct/25/aids.china
http://www.theguardian.com/world/2003/dec/01/gender.uk
sexual health UK
http://www.theguardian.com/uk/2007/nov/23/aids.world
http://www.guardian.co.uk/society/2007/nov/23/health
http://commentisfree.guardian.co.uk/deborah_jack/2007/11/
still_with_us.html
AIDS vaccine USA
https://www.npr.org/sections/goatsandsoda/2023/01/26/
1150851465/why-inventing-a-vaccine-for-aids-is-tougher-than-for-covid
http://www.nytimes.com/2015/02/19/
health/new-approach-to-blocking-hiv-raises-talk-of-an-aids-vaccine.html
http://www.nytimes.com/2009/10/19/
opinion/19berkley.html
vaginal microbicide
USA
http://www.nytimes.com/2010/09/04/world/africa/
04safrica.html
treatment
USA
http://www.nytimes.com/2012/11/21/world/
new-hiv-cases-falling-in-some-poor-nations-but-treatment-still-lags.html
take the
medicine
drug > injection > Cabenuva
one of a new type of anti-AIDS drugs
that need to be taken only a few times a year.
https://www.npr.org/sections/goatsandsoda/2020/11/19/
936627318/long-lasting-anti-aids-meds-eliminate-psychic-toll-of-daily-pill
antiretroviral drugs
USA
https://www.npr.org/2015/08/16/
432435481/though-not-a-death-sentence-hiv-aids-still-holds-a-powerful-stigma
AIDS
prevention USA
https://www.nytimes.com/2015/10/25/
nyregion/dr-beny-primm-pioneer-in-aids-prevention-dies-at-87.html
prevent AIDS > Truvada
Truvada,
a daily pill that has been shown
to prevent infection with the virus
that causes AIDS.
https://www.npr.org/sections/health-shots/2018/06/30/
624045995/rising-cost-of-prep-a-pill-that-prevents-hiv-pushes-it-out-of-reach-for-many
http://www.npr.org/blogs/health/2015/03/11/
392362374/would-a-pill-to-protect-teens-from-hiv-make-them-feel-invincible
http://www.theguardian.com/society/2015/feb/24/
daily-pill-truvada-cuts-spread-of-hiv-by-86-study-shows
http://www.nytimes.com/2014/07/04/upshot/
pill-to-prevent-hiv-gets-a-prominent-backer-andrew-cuomo.html
http://www.nytimes.com/2014/05/15/health/
advocating-pill-us-signals-shift-to-prevent-aids.html
http://www.nytimes.com/roomfordebate/2014/06/17/
is-prep-a-good-way-to-fight-hiv-infections
AIDS Scientists Encouraged
By Antibodies That Hit
Monkey Virus USA
31 October 2013
http://www.npr.org/blogs/health/2013/10/31/
242093426/aids-scientists-encouraged-by-antibodies-that-hit-monkey-virus
William Herman Prusof USA 1920-2011
pharmacologist
at the Yale School of Medicine
who, with a
colleague,
developed an effective component
in the first generation of drug cocktails
used
to treat AIDS
http://www.nytimes.com/2011/04/07/
health/research/07prusoff.html
UCLA Louise M. Darling
Biomedical Library
History and Special Collections Division > AIDS Posters
https://digital.library.ucla.edu/catalog/ark:/21198/zz0002ksb2
2021 > TV series > It's a Sin
UK
https://www.npr.org/2021/02/17/
968365774/its-a-sin-series-set-during-aids-epidemic-resonates-during-covid-19
https://www.theguardian.com/news/audio/2021/feb/15/
its-a-sin-nurse-reflects-on-aids-crisis-1980s-podcast
https://www.theguardian.com/tv-and-radio/2021/feb/10/
its-a-sin-there-is-such-a-raw-truth-to-it
https://www.theguardian.com/tv-and-radio/2021/jan/22/
its-a-sin-review-russell-t-davies-queer-as-folk-aids-channel-4
https://www.theguardian.com/tv-and-radio/2021/jan/09/
its-a-sin-its-not-about-death-its-about-vibrant-beautiful-lives
Corpus of news articles
Health > Viruses > H.I.V. >
Syndrom > AIDS
Early Treatment Is Found
to Clear H.I.V. in a 2nd Baby
MARCH 5, 2014
The New York Times
By DONALD G. McNEIL Jr.
BOSTON — When scientists made the stunning announcement last
year that a baby born with H.I.V. had apparently been cured through aggressive
drug treatment just 30 hours after birth, there was immediate skepticism that
the child had been infected in the first place.
But on Wednesday, the existence of a second such baby was revealed at an AIDS
conference here, leaving little doubt that the treatment works. A leading
researcher said there might be five more such cases in Canada and three in South
Africa.
And a clinical trial in which up to 60 babies who are born infected will be put
on drugs within 48 hours is set to begin soon, another researcher added.
If that trial works — and it will take several years of following the babies to
determine whether it has — the protocol for treating all 250,000 babies born
infected each year worldwide will no doubt be rewritten.
“This could lead to major changes, for two reasons,” said Dr. Anthony S. Fauci,
executive director of the National Institute for Allergy and Infectious
Diseases. “Both for the welfare of the child, and because it is a huge proof of
concept that you can cure someone if you can treat them early enough.”
The announcement was the third piece of hopeful news in two days about the virus
that causes AIDS.
On Tuesday, scientists reported that injections of long-lasting AIDS drugs
fended off infection in monkeys, and on Wednesday, researchers announced a “gene
editing” advance that might enable immune cells to repel the virus.
The first infant to make an apparent recovery from H.I.V. infection, now famous
as the “Mississippi baby,” was described last March at the Conference on
Retroviruses and Opportunistic Infections, the same annual meeting where the new
case was reported on Wednesday.
The Mississippi child, now more than 3 years old, is still virus-free, said Dr.
Deborah Persaud, a virologist who has run ultrasensitive tests on both children
in her lab at the Johns Hopkins Children’s Center in Baltimore.
The second baby, a girl born at Miller Children’s Hospital in Long Beach,
Calif., is now 9 months old and apparently free of the virus that causes AIDS.
Her mother, who has advanced AIDS and is mentally ill, arrived in labor; she had
been prescribed drugs to protect her baby but had not taken them.
Four hours after the birth, a pediatrician, Dr. Audra Deveikis, drew blood for
an H.I.V. test and immediately started the baby on three drugs — AZT, 3TC and
nevirapine — at the high doses usually used for treatment of the virus.
The normal preventive regimen for newborns would be lower doses of two drugs;
doctors usually do not use the more aggressive treatment until they are sure the
baby is infected, and then sometimes not in the first weeks.
“Of course I had worries,” Dr. Deveikis said in an interview here. “But the
mother’s disease was not under control, and I had to weigh the risk of
transmission against the toxicity of the meds.”
“I’d heard of the Mississippi baby, I’d watched the video,” she added. “I knew
that if you want to prevent infection, early treatment is critical.”
The Long Beach baby is now in foster care, she said. The mother is still alive
as well.
It is incorrect to describe the baby as “cured” or even as “in remission”
because she is still on the drugs, Dr. Persaud said. But because the most
sensitive blood tests can find no virus capable of replicating, she describes
the baby as “having sero-reverted to H.I.V.-negative.”
Both DNA and RNA of the virus were found in the baby’s early blood and spinal
fluid samples, so Dr. Persaud said it was virtually certain she was infected at
birth. The virus began to disappear six days after birth and was undetectable
within 11 days.
It is considered medically unethical to stop the baby’s drugs now, but Dr.
Deveikis and Dr. Yvonne J. Bryson, a pediatric AIDS expert at the University of
California, Los Angeles, who is also working on the case, said they would
consider stopping them briefly to see what happens if the baby is still
virus-free at age 2.
Dr. Bryson is one of three investigators who will lead the clinical trial
seeking 60 babies.
Obstetricians and pediatricians in the United States, South Africa and Brazil
will be alerted to watch for babies being born to mothers who have not taken
drugs to prevent mother-child transmission and to get them on full
antiretroviral treatment immediately, even before the first blood test has been
finished. (In the United States, fewer than 200 children each year are born with
H.I.V.)
The trial will be funded by Dr. Fauci’s institute and be part of the Impact
series of trials concentrating on preventing viral transmission to newborns.
“When we described the Mississippi baby, we were met with some skepticism,” she
said. The Long Beach baby “was definitely infected.”
The Mississippi baby was born to a mother who got no prenatal care and was
unaware that she was infected. Worried doctors at a local hospital transferred
the baby to the University of Mississippi Medical Center, where a pediatrician,
Dr. Hannah B. Gay, started aggressive antiretroviral treatment about 30 hours
after birth.
Then, 18 months later, the mother stopped taking the baby to appointments and
stopped giving the drugs. Five months later, when she came to an appointment,
doctors feared the baby would be teeming with virus.
Instead, to their astonishment, they found none. And Dr. Persaud’s testing has
found none, despite using tests normally able to detect dormant virus in adult
patients on successful treatment.
Although antiretrovirals prevent the virus from replicating, a small amount
usually persists in reservoirs throughout the body, integrated into the DNA of
cells. Dr. Persaud’s test can activate those cells and force them to “spit out”
the virus, where it can be detected.
Dr. Steven G. Deeks, an AIDS expert at the University of California, San
Francisco, said the Long Beach baby offered more convincing evidence that
starting therapy virtually at birth seems to kill the virus before it
establishes a permanent reservoir.
“But it sure would be nice to have a way to decide when to stop” the treatment,
he added. “That’s the next question.”
A version of this article appears in print
on March 6, 2014,
on page A1 of the New York edition with the headline:
Early Treatment Found to Clear H.I.V. in 2nd Baby.
Early Treatment Is Found to Clear H.I.V. in
a 2nd Baby,
NYT,
5.3.2014,
https://www.nytimes.com/2014/03/06/
health/second-success-raises-hope-for-a-way-to-rid-babies-of-hiv.html
In
Medical First,
a Baby With H.I.V.
Is Deemed Cured
March 3,
2013
The New York Times
By ANDREW POLLACK
and DONALD G. McNEIL Jr.
Doctors
announced on Sunday that a baby had been cured of an H.I.V. infection for the
first time, a startling development that could change how infected newborns are
treated and sharply reduce the number of children living with the virus that
causes AIDS.
The baby, born in rural Mississippi, was treated aggressively with
antiretroviral drugs starting around 30 hours after birth, something that is not
usually done. If further study shows this works in other babies, it will almost
certainly be recommended globally. The United Nations estimates that 330,000
babies were newly infected in 2011, the most recent year for which there is
data, and that more than three million children globally are living with H.I.V.
If the report is confirmed, the child born in Mississippi would be only the
second well-documented case of a cure in the world. That could give a lift to
research aimed at a cure, something that only a few years ago was thought to be
virtually impossible, though some experts said the findings in the baby would
probably not be relevant to adults.
The first person cured was Timothy Brown, known as the Berlin patient, a
middle-aged man with leukemia who received a bone-marrow transplant from a donor
genetically resistant to H.I.V. infection.
“For pediatrics, this is our Timothy Brown,” said Dr. Deborah Persaud, associate
professor at the Johns Hopkins Children’s Center and lead author of the report
on the baby. “It’s proof of principle that we can cure H.I.V. infection if we
can replicate this case.”
Dr. Persaud and other researchers spoke in advance of a presentation of the
findings on Monday at the Conference on Retroviruses and Opportunistic
Infections in Atlanta. The results have not yet been published in a
peer-reviewed medical journal.
Some outside experts, who have not yet heard all the details, said they needed
convincing that the baby had truly been infected. If not, this would be a case
of prevention, something already done for babies born to infected mothers.
“The one uncertainty is really definitive evidence that the child was indeed
infected,” said Dr. Daniel R. Kuritzkes, chief of infectious diseases at Brigham
and Women’s Hospital in Boston.
Dr. Persaud and some other outside scientists said they were certain the baby —
whose name and gender were not disclosed — had been infected. There were five
positive tests in the baby’s first month of life — four for viral RNA and one
for DNA. And once the treatment started, the virus levels in the baby’s blood
declined in the pattern characteristic of infected patients.
Dr. Persaud said there was also little doubt that the child experienced what she
called a “functional cure.” Now 2 1/2, the child has been off drugs for a year
with no sign of functioning virus.
The mother arrived at a rural hospital in the fall of 2010 already in labor and
gave birth prematurely. She had not seen a doctor during the pregnancy and did
not know she had H.I.V. When a test showed the mother might be infected, the
hospital transferred the baby to the University of Mississippi Medical Center,
where it arrived at about 30 hours old.
Dr. Hannah B. Gay, an associate professor of pediatrics, ordered two blood draws
an hour apart to test for the presence of the virus’ RNA and DNA.
The tests found a level of virus at about 20,000 copies per milliliter, fairly
low for a baby. But since tests so early in life were positive, it suggests the
infection occurred in the womb rather than during delivery, Dr. Gay said.
Typically a newborn with an infected mother would be given one or two drugs as a
prophylactic measure. But Dr. Gay said that based on her experience, she almost
immediately used a three-drug regimen aimed at treatment, not prophylaxis, not
even waiting for the test results confirming infection.
Virus levels rapidly declined with treatment and were undetectable by the time
the baby was a month old. That remained the case until the baby was 18 months
old, after which the mother stopped coming to the hospital and stopped giving
the drugs.
When the mother and child returned five months later, Dr. Gay expected to see
high viral loads in the baby. But the tests were negative.
Suspecting a laboratory error, she ordered more tests. “To my greater surprise,
all of these came back negative,” Dr. Gay said.
Dr. Gay contacted Dr. Katherine Luzuriaga, an immunologist at the University of
Massachusetts, who was working with Dr. Persaud and others on a project to
document possible pediatric cures. The researchers, sponsored by amfAR, the
Foundation for AIDS Research, put the baby through a battery of sophisticated
tests. They found tiny amounts of some viral genetic material but no virus able
to replicate, even lying dormant in so-called reservoirs in the body.
There have been scattered cases reported in the past, including one in The New
England Journal of Medicine in 1995, of babies clearing the virus, even without
treatment.
Those reports were greeted skeptically, particularly since testing methods were
not very sophisticated back then. But those reports and this new one could
suggest there is something different about babies’ immune systems, said Dr.
Joseph McCune of the University of California, San Francisco.
One hypothesis is that the drugs killed off the virus before it could establish
a hidden reservoir in the baby. One reason people cannot be cured now is that
the virus hides in a dormant state, out of reach of existing drugs. When drug
therapy is stopped, the virus can emerge from hiding.
“That goes along with the concept that, if you treat before the virus has had an
opportunity to establish a large reservoir and before it can destroy the immune
system, there’s a chance you can withdraw therapy and have no virus,” said Dr.
Anthony S. Fauci, the director of the National Institute for Allergy and
Infectious Diseases. Adults, however, typically do not know they are infected
right as it happens, he said.
Dr. Steven Deeks, professor of medicine at the University of California, San
Francisco, said if the reservoir never established itself, then he would not
call it a true cure, though this was somewhat a matter of semantics. “Was there
enough time for a latent reservoir, the true barrier to cure, to establish
itself?” he said.
Still, he and others said, the results could lead to a new protocol for quickly
testing and treating infants.
In the United States, transmission from mother to child is rare — several
experts said there are only about 200 cases a year or even fewer — because
infected mothers are generally treated during their pregnancies.
If the mother has been treated during pregnancy, babies are typically given six
weeks of prophylactic treatment with one drug, AZT, while being tested for
infection. In cases like the Mississippi one, where the mother was not treated
during pregnancy, standards have been changing, but typically two drugs are
used.
But women in many developing countries are less likely to be treated during
pregnancy. And in South Africa and other African countries that lack
sophisticated testing, babies born to infected mothers are often not tested
until after six weeks, said Dr. Yvonne Bryson, chief of global pediatric
infectious disease at the University of California, Los Angeles.
Dr. Bryson, who was not involved in the Mississippi work, said she was certain
the baby had been infected and called the finding “one of the most exciting
things I’ve heard in a long time.”
Studies are being planned to see if early testing and aggressive treatment can
work for other babies. While the bone marrow transplant that cured Mr. Brown is
an arduous and life-threatening procedure, the Mississippi treatment is not and
could become a new standard of care.
While it might be difficult for some poorer countries to do, treating for only a
year or two would be cost effective, “sparing the kid a lifetime of
antiretroviral therapy,” said Rowena Johnston, director of research at amfAR.
In Medical First, a Baby With H.I.V. Is Deemed Cured,
NYT, 3.3.3013,
http://www.nytimes.com/2013/03/04/health/
for-first-time-baby-cured-of-hiv-doctors-say.html
New H.I.V. Cases
Falling in Some Poor Nations,
but Treatment Still Lags
November 20, 2012
The New York Times
By DONALD G. McNEIL Jr.
New infections with H.I.V. have dropped by half in the past decade in 25 poor
and middle-income countries, many of them in Africa, the continent hardest hit
by AIDS, the United Nations said Tuesday.
The greatest success has been in preventing mothers from infecting their babies,
but focusing testing and treatment on high-risk groups like gay men, prostitutes
and drug addicts has also paid dividends, said Michel Sidibé, the executive
director of the agency U.N.AIDS.
“We are moving from despair to hope,” he said.
Despite the good news from those countries, the agency’s annual report showed
that globally, progress is steady but slow. By the usual measure of whether the
fight against AIDS is being won, it is still being lost: 2.5 million people
became infected last year, while only 1.4 million received lifesaving treatment
for the first time.
“There has been tremendous progress over the last decade, but we’re still not at
the tipping point,” said Mitchell Warren, the executive director of AVAC, an
advocacy group for AIDS prevention. “And the big issue, sadly, is money.”
Some regions, like Southern Africa and the Caribbean, are doing particularly
well, while others, like Eastern Europe, Central Asia and the Middle East, are
not. Globally, new infections are down 22 percent from 2001, when there were 3.2
million. Among newborns, they fell 40 percent, to 330,000 from 550,000.
The two most important financial forces in the fight, the multinational Global
Fund for AIDS, Tuberculosis and Malaria and the domestic President’s Emergency
Plan for AIDS Relief, were both created in the early 2000s and last year
provided most of the $16.8 billion spent on the disease. But the need will soon
be $24 billion a year, the groups said.
“Where is that money going to come from?” Mr. Warren asked.
The number of people living with H.I.V. rose to a new high of 34 million in
2011, while the number of deaths from AIDS was 1.7 million, down from a peak of
2.3 million in 2005. As more people get life-sustaining antiretroviral
treatment, the number of people living with H.I.V. grows.
Globally, the number of people on antiretroviral drugs reached 8 million, up
from 6.6 million in 2010. However, an additional 7 million are sick enough to
need them. The situation is worse for children; 72 percent of those needing
pediatric antiretrovirals do not get them.
New infections fell most drastically since 2001 in Southern Africa — by 71
percent in Botswana, 58 percent in Zambia and 41 percent in South Africa, which
has the world’s biggest epidemic.
But countries with drops greater than 50 percent were as geographically diverse
as Barbados, Cambodia, the Dominican Republic, Ethiopia, India and Papua New
Guinea.
The most important factor, Mr. Sidibé said, was not nationwide billboard
campaigns to get people to use condoms or abstain from sex. Nor was it male
circumcision, a practice becoming more common in Africa.
Rather, it was focusing treatment on high-risk groups. While saving babies is
always politically popular, saving gay men, drug addicts and prostitutes is not,
so presidents and religious leaders often had to be persuaded to help them. Much
of Mr. Sidibé’s nearly four years in his post has been spent doing just that.
Many leaders are now taking “a more targeted, pragmatic approach,” he said, and
are “not blocking people from services because of their status.”
Fast-growing epidemics are often found in countries that criminalize behavior.
For example, homosexuality is illegal in many Muslim countries in the Middle
East and North Africa, so gay and bisexual men, who get many of the new
infections, cannot admit being at risk. The epidemics in Eastern Europe and
Central Asia are driven by heroin, and in those countries, methadone treatment
is sometimes illegal.
Getting people on antiretroviral drugs makes them 96 percent less likely to
infect others, studies have found, so treating growing numbers of people with
AIDS has also helped prevent new infections.
Ethiopia’s recruitment of 35,000 community health workers, who teach young
people how to protect themselves, has also aided in prevention.
Mr. Sidibé acknowledged that persuading rich countries to keep donating money
was a struggle. The Global Fund is just now emerging from a year of turbulence
with a new executive director, and the American program has come under budget
pressures. Also, he noted, many countries like South Africa and China are
relying less on donors and are paying their own costs. The number of people on
treatment in China jumped 50 percent in a single year.
Mr. Warren’s organization said in a report on Tuesday that the arsenal of
prevention methods had expanded greatly since the days when the choice was
abstain from sex, be faithful or use condoms. Male circumcision, which cuts
infection risk by about 60 percent, a daily prophylactic pill for the uninfected
and vaginal microbicides for women are in use or on the horizon, and countries
need to use the ones suited to their epidemics, the report concluded.
New H.I.V. Cases Falling in Some Poor Nations, but Treatment Still Lags,
NYT,
20.11.2012,
http://www.nytimes.com/2012/11/21/world/
new-hiv-cases-falling-in-some-poor-nations-but-treatment-still-lags.html
Imagine a World Without AIDS
July 27, 2012
The New York Times
By DANIELLE OFRI
THE beginning of the end of AIDS? The article with that title jumped out at me
last week, as I did my weekly table-of-contents scan of The New England Journal
of Medicine. I wasn’t prepared for the flood of emotion that overcame me. The
beginning of the end? Could it really be?
For those of us who did our medical training in the late ’80s and early ’90s,
AIDS saturated our lives. The whole era had a medieval feel, with visceral
suffering and human decimation all around. Death was vivid, brutal and
omnipresent.
Bellevue Hospital, where I trained, was one of those city hospitals that felt
like ground zero for the plague. Every third admission seemed to be a patient in
his mid-20s who looked as if he’d arrived from Dachau or Biafra, with nary a
T-cell to his name. Horrific Kaposi’s sarcoma ulcerated these patients’ bodies.
P.C.P., a brutal form of pneumonia, strangled their breathing. Fevers and
infections plundered every organ system. What few defenses their bodies mustered
were pummeled into insignificance.
The utter relentlessness of the disease pummeled the doctors-in-training as
well. It felt as if we were slogging knee-deep in death, with a horizon that was
a monochrome of despair. Witnessing your own generation dying off is not for the
faint of heart.
The 17 West AIDS ward in Bellevue was always full to capacity, so H.I.V.
patients overflowed into the general medical wards, and of course swamped the
prison ward, the tuberculosis ward, the pediatric ward and the emergency room.
We even had a “spillover” ward, 12 East, reserved for the “actively dying.” The
hospital had carved out a ward of private rooms — otherwise unheard-of in a city
hospital — so that these patients could have a modicum of privacy in their final
days. Needless to say, 12 East was also full to capacity, with a line of
patients waiting for a room to “open up.”
If you’d grabbed a random intern toward the end of my residency in 1995, and
asked her if she could envision the headline “The Beginning of the End of AIDS”
in less than 20 years, she would have simply stared uncomprehendingly at you
with bleary eyes. More than 50,000 Americans died of AIDS that year. By 2009,
the number had edged under 20,000.
In the worlds of both medicine and metaphor, the narrative arc of AIDS has
almost no peer. The transformation from hopelessness to pragmatic optimism is —
scientifically speaking — nothing short of miraculous. Potent combinations of
antiviral medications that brought patients off their deathbeds and back to
life, viral load testing and H.I.V. genotyping that helped tailor treatment
regimens, screening of the blood supply, aggressive public health campaigns,
prevention of maternal-fetal transmission — we could hardly have envisioned the
pace of development.
After years of disappointments, H.I.V. vaccine research is heating up again, as
breakthroughs in the understanding of H.I.V. immunology have identified nearly
two dozen potential vaccine candidates. The apparent H.I.V. cure as a result of
a bone-marrow transplant in a man known as the “Berlin patient” has stimulated
tantalizing gene therapy research.
The staggering progress of these past two decades leaves me breathless, and to
be honest, almost teary-eyed. For nearly every other category of disease that
afflicts my patients, the treatments are largely the same as when I was an
intern. Yes, we have fancier stents for our cardiac patients, and more targeted
chemotherapy for our cancer patients, but the overall paradigms have shifted
only incrementally.
H.I.V. has been easier to target, in part, because it is caused by a single
infectious agent — as opposed to the diverse factors that influence
cardiovascular disease and cancer. And then there was the avalanche of resources
and the galvanizing of public activism that served to concentrate scientific
efforts in a manner never seen before. By no means do I wish to belittle the
impressive advances in other fields of medicine, but our oncology wards and
cardiac wards still do a brisk business.
AIDS patients in the hospital are a rarity now — they are more likely to be
admitted for an ulcer or a heart attack than for an H.I.V.-related illness. The
overwhelming majority receive their medical care in outpatient settings, like
everyone else who is living with a disease rather than dying of a disease. AIDS
has settled in next to hypertension and diabetes as one of those chronic
conditions that patients deal with over the course of a lifetime.
“Over the course of a lifetime.” Now there’s a concept we never thought about
back then.
There is still a long way to go, of course. The 19th annual International AIDS
Conference just ended on Friday, and no one is underestimating the gravity of
the challenges that remain, particularly in developing countries. But to even
contemplate, however tentatively, the beginning of the end is something that my
peers and I never imagined happening in our lifetimes.
I often think about grim days we spent doing rounds on 17 West and 12 East. I
remember the slow and tortured deaths of our patients, their emaciated bodies
disintegrating into nothingness before our eyes. More tears were shed on those
wards than any I’ve worked in since.
And what happened? The 17 West AIDS ward became a regular medical ward. The 12
East dying ward was turned into offices. And then, this month, the inpatient
AIDS service at Bellevue closed down entirely. If that doesn’t signify the
beginning of the end, I don’t know what does.
Danielle Ofri, an associate professor
at New York University School of Medicine,
is the editor of the Bellevue Literary Review
and the author, most recently,
of “Medicine in Translation:
Journeys With My Patients.”
Imagine a World Without AIDS, NYT, 27.7.2012,
http://www.nytimes.com/2012/07/28/opinion/imagine-a-world-without-aids.html
The
Long, Uphill Battle Against AIDS
July 27,
2012
The New York Times
The
international AIDS conference in Washington has already made two points clear.
There is no prospect that scientists will any time soon find the ultimate
solutions to the AIDS epidemic, namely a vaccine that would prevent infection
with the AIDS virus or a “cure” for people already infected with the virus. Even
so, health care leaders already have many tools that have been shown in rigorous
trials to prevent transmission of the virus, making it feasible to talk of
controlling the epidemic within the foreseeable future. The only question is
whether the nations of the world are willing to put up enough money and make the
effort to do it.
An estimated 34.2 million people around the world are currently infected with
H.I.V., the virus that causes AIDS. According to the United Nations agency that
tracks the disease, some 23.5 million of these live in sub-Saharan Africa and
another 4.2 million in India and Southeast Asia. About 1.1 million live in the
United States.
This conference is the first in more than two decades to be held in the United
States. It became possible only when a benighted policy that prohibited entry
visas for people suffering from AIDS or infected with H.I.V. was finally
overturned in 2009. It was “a bad policy, based on faulty science, that ran
contrary to America’s deepest values,” Kathleen Sebelius, the secretary of
health and human services, told the conference.
There has been optimistic talk at the conference about accelerating the search
for a “cure” that would allow people to eventually stop taking the drugs that
have prolonged many lives for decades — and about developing a truly effective
vaccine. But Dr. Anthony Fauci, the American government’s top AIDS expert, made
clear just how difficult those tasks will be. He told the conference that a cure
was “way upstream” and depends on future research breakthroughs, and he called
the most successful vaccine trial to date “humbling” because it showed only a
modest degree of efficacy.
Instead of waiting for these future possibilities, Dr. Fauci and other health
leaders are proposing the broad adoption of other available tools to reduce the
spread of the virus so as to produce an “AIDS-free generation,” a goal
enunciated last year by Secretary of State Hillary Rodham Clinton. In her talk
at the conference this week, Mrs. Clinton anticipated a time when virtually no
child anywhere would be born with the virus, teenagers and young adults would
have much less risk of becoming infected and those that do become infected would
have access to treatments to prevent them from developing full-fledged AIDS or
passing the virus on to others.
She cited the importance of condoms, counseling and testing; voluntary
circumcision to protect males from becoming infected by a female partner;
treating mothers to prevent transmission to their babies; and treating infected
people with antiviral drugs as early as possible to enhance their own health and
lessen the likelihood they will spread the virus to others. Studies also show
that people at high risk of infection can protect themselves by taking an
antiviral pill daily.
All that will take money. There is a widespread misconception that donors from
well-heeled international organizations, rich countries and charitable
foundations are the main source of money to combat the global epidemic. The
share provided by international donors has, in fact, stagnated while the share
provided by low- and middle-income countries to fight the epidemic on their own
turf has been growing rapidly. Last year, the poorer countries invested $8.6
billion of their own money while international financing remained at $8.2
billion, the 2008 level, according to a report from the United Nations AIDS
agency. Both groups will need to expand their contributions to meet ambitious
treatment and prevention goals set for coming years.
Mrs. Clinton announced additional financing for AIDS programs, but perhaps her
most important pledge was that the United States will issue a blueprint by Dec.
1 setting forth a road map for how to achieve an AIDS-free generation. To be
effective, it will need to set priorities and define specific health outcomes
and coverage targets and require detailed annual reports on the progress being
made. It is unacceptable that millions of people sick enough to need treatment
are not getting it.
The Long, Uphill Battle Against AIDS, NYT, 27.7.2012,
http://www.nytimes.com/2012/07/28/opinion/
the-long-uphill-battle-against-aids.html
A Decade
of Progress on AIDS
November
30, 2011
The New York Times
By BONO
I’LL tell
you the worst part about it, for me.
It was the look in their eyes when the nurses gave them the diagnosis —
H.I.V.-positive — then said there was no treatment. I saw no anger in their
expression. No protest. If anything, just a sort of acquiescence.
The anger came from the nurses, who knew there really was a treatment — just not
for poor people in poor countries. They saw the absurdity in the fact that an
accident of geography would deny their patients the two little pills a day that
could save their lives.
This was less than a decade ago. And all of us who witnessed these dedicated
African workers issuing death sentence after death sentence still feel fury and
shame. AIDS set off an almost existential crisis in the West. It forced us to
ask ourselves the big, uncomfortable questions, like whether capitalism, which
invented the global village and kept it well stocked with stuff, could also
create global solutions. Whether we were interested in charity... or justice.
The wanton loss of so many lives in Africa offended the very idea of America:
the idea that everyone is created equal and that your destiny is your own to
make. By the late 1990s, AIDS campaigners in the United States and around the
world teamed up with scientists and doctors to insist that someone — anyone —
put the fire out. The odds against this were as extreme as the numbers: in 2002,
two million people were dying of AIDS and more than three million were newly
infected with H.I.V. Around 50,000 people in the sub-Saharan region had access
to treatment.
Yet today, here we are, talking seriously about the “end” of this global
epidemic. There are now 6.6 million people on life-saving AIDS medicine. But
still too many are being infected. New research proves that early antiretroviral
treatment, especially for pregnant women, in combination with male circumcision,
will slash the rate of new H.I.V. cases by up to 60 percent. This is the tipping
point we have been campaigning for. We’re nearly there.
How did we get here? America led. I mean really led.
The United States performed the greatest act of heroism since it jumped into
World War II. When the history books are written, they will show that millions
of people owe their lives to the Yankee tax dollar, to just a fraction of an aid
budget that is itself less than 1 percent of the federal budget.
For me, a fan and a pest of America, it’s a tale of strange bedfellows: the gay
community, evangelicals and scruffy student activists in a weird sort of
harmony; military men calling AIDS in Africa a national security issue; the
likes of Nancy Pelosi, Barbara Lee and John Kerry in lock step with Bill Frist
and Rick Santorum; Jesse Helms, teary-eyed, arriving by walker to pledge support
from the right; the big man, Patrick Leahy, offering to punch out a cranky
Congressional appropriator; Jeffrey Sachs, George Soros and Bill Gates, backing
the Global Fund to Fight AIDS, Tuberculosis and Malaria; Rupert Murdoch (yes,
him) offering the covers of the News Corporation.
Also: a conservative president, George W. Bush, leading the largest ever
response to the pandemic; the same Mr. Bush banging his desk when I complained
that the drugs weren’t getting there fast enough, me apologizing to Mr. Bush
when they did; Bill Clinton, arm-twisting drug companies to drop their prices;
Hillary Rodham Clinton, making it policy to eradicate the transmission of H.I.V.
from mother to child; President Obama, who is expected to make a game changing
announcement this World AIDS Day to finish what his predecessors started — the
beginning of the end of AIDS.
And then there were the everyday, every-stripe Americans. Like a tattooed
trucker I met off I-80 in Iowa who, when he heard how many African truck drivers
were infected with H.I.V., told me he’d go and drive the pills there himself.
Thanks to them, America led. Really led.
This was smart power. Genius, really. In 2007, 8 out of the 10 countries in the
world that viewed the United States most fondly were African. And it can’t be a
bad thing for America to have friends on a continent that is close to half
Muslim and that, by 2025, will surpass China in population.
Activists are a funny lot. When the world suddenly starts marching in step with
us, we just point out with (self-)righteous indignation all that remains to be
done. But on this World AIDS Day I would like you to stop and consider what
America has achieved in this war to defend lives lived far away and sacred
principles held closer to home.
The moonshot, I know, is a tired metaphor; I’ve exhausted it myself. But
America’s boldest leap of faith is worth recalling. And the thing is, as I see
it, the Eagle hasn’t landed yet. Budget cuts ... partisan divisions ... these
put the outcome in jeopardy just as the science falls into place. To get this
far and not plant your flag would be one of the greatest accidental evils of
this recession.
Bono is the
lead singer of the band U2
and a founder
of the advocacy group ONE
and the (Product)RED campaign.
A Decade of Progress on AIDS, NYT, 30.11.2011,
http://www.nytimes.com/2011/12/01/opinion/a-decade-of-progress-on-aids.html
30 years on,
AIDS fight may tilt more to treatment
CHICAGO/GENEVA | Fri Jun 3, 2011
1:30am EDT
Reuters
By Julie Steenhuysen and Barbara Lewis
CHICAGO/GENEVA (Reuters) - After 30 years of AIDS prevention efforts, global
leaders may now need to shift their focus to spending more on drugs used to
treat the disease as new data show this is also the best way to prevent the
virus from spreading.
The U.N. General Assembly will take up the issue next week as it assesses
progress in fighting the disease -- first reported on June 5, 1981 -- that has
infected more than 60 million people and claimed nearly 30 million lives.
Guiding the meeting is groundbreaking new data that shows early treatment of the
human immunodeficiency virus, or HIV, can cut its transmission to a sexual
partner by 96 percent.
"There had been for a long time this artificial dichotomy or artificial tension
between treatment versus prevention. Now it is very clear that treatment is
prevention and treatment is an important part of a multifaceted combination
strategy," Dr. Anthony Fauci, director of the National Institute of Allergy and
Infectious Diseases division of the National Institutes of Health (NIH), told
Reuters.
Fauci, who has made AIDS research his life's work, has a big role to play in the
discussion of the NIH-funded study made public on May 12.
"A month ago, we didn't have that data. People were still arguing. 'Well, we are
not so sure if you treat people you are really going to prevent infection,'"
Fauci said. "The policy makers need to sit down and say, 'Now that we know this,
is this going to be enough incentive to change around our policy?'"
That could mean redirecting, or adding to, global spending on fighting AIDS,
particularly how much is spent on education or other research versus
antiretroviral drugs that allow patients to live with the suppressed disease for
many years.
In 2010, nearly $16 billion was spent on HIV response in low and middle-income
countries, according to the U.N. Program on HIV/AIDS.
UNAIDS says at least $22 billion will be needed to combat the disease by 2015,
helping avert 12 million new infections and 7.4 million more deaths in the next
decade.
Globally, the number of people living with HIV rose to 34 million by the end of
2010, from 33.3 million a year earlier. But in poorer countries, a majority of
eligible patients were not receiving antiretroviral treatment, according to
UNAIDS.
Fauci says he has already discussed this with policymakers and may make public
his views on needed policy changes at the International AIDS Society meeting in
Rome.
"I don't think it's going to be one-size-fits all," Fauci said of the policy
approach. "There is going to be certainly a difference between how things are
looked at in the developing world and the developed world. And within the
developed world, I think it will be a country-by-country issue."
UNAIDS Executive Director Michel Sidibe noted that AIDS remained "a metaphor for
inequality" as the vast majority of patients live in Africa, where every year
nearly 400,000 babies are born with HIV.
"If you're privileged to be born in the North, you will not die from HIV. It
you're privileged to be born in the North, you will not have a baby born with
HIV," Sidibe said.
"Countries need to start looking at innovative financing. We need to have drugs
which are not just for the rich market."
(Writing by Michele Gershberg; Editing by Jackie Frank)
30 years on, AIDS fight may tilt more to treatment, R,
3.6.2011,
http://www.reuters.com/article/2011/06/03/us-aids-policy-idUSTRE7520RQ20110603
Factbox:
HIV/AIDS numbers
from around the world
Wed Jun 1, 2011
9:03am EDT
Reuters
(Reuters) - Here are some global data on HIV and AIDS
from the latest update report by the Joint U.N. Program on
HIV/AIDS (UNAIDS).
THE GLOBAL PICTURE:
* An estimated 33.3 million people worldwide had the human immunodeficiency
virus (HIV) that causes AIDS in 2009, according to the latest figures issued by
(UNAIDS). There were 26.2 million in 1999.
* There were an estimated 1.8 million AIDS-related deaths around the world in
2009.
* One in four AIDS deaths is caused by tuberculosis, a preventable and curable
disease.
* Since the AIDS pandemic started in the early 1980s, more than 60 million
people have been infected with HIV and nearly 30 million have died of
HIV-related causes.
* In 2009, there were 2.6 million new HIV infections, down from 3.1 million in
1999.
* Around 370,000 children were born with HIV in 2009, bringing to 2.5 million
the total number of children under 15 living with HIV.
*
AFRICA & ASIA:
* An estimated 1.8 million people were newly infected with HIV in sub-Saharan
Africa in 2009, bringing to 22.5 million the number of Africans who have HIV.
* There were 1.3 million AIDS-related deaths in Sub-Saharan Africa in 2009.
* Out of the total number of people living with HIV worldwide in 2009, 34
percent resided in 10 countries of Southern Africa.
* With an estimated 5.6 million HIV-positive people, South Africa continues to
have the world's largest HIV epidemic. Swaziland has the highest adult HIV
prevalence in the world: an estimated 25.9 percent of people in the country were
living with HIV in 2009.
* In Asia an estimated 4.9 million people were living with HIV in 2009, about
the same number as five years earlier.
* An estimated 300,000 people died from AIDS-related causes in 2009 compared to
250,000 in 2001.
* An estimated 360,000 people were newly infected with HIV in 2009, compared to
450,000 in 2001, a 20 percent reduction over eight years. In India, Nepal and
Thailand, the incidence rate of new HIV infections fell by more than 25 percent
between 2001 and 2009.
OTHER REGIONS:
* Some 1.5 million people in Eastern Europe and Central Asia have HIV.
* In Central and South America, new HIV infections were an estimated 92,000 in
2009, bringing to 1.4 million the number of people there who have HIV. An
estimated 68,000 people died of AIDS-related illnesses there in 2009.
* There were around 2.3 million people with HIV in North America and western and
central Europe in 2009 and there were 101,000 new HIV infections in that year.
SOURCE: UNAIDS/Reuters
(Compiled by David Cutler,
London Editorial Reference Unit;)
Factbox: HIV/AIDS numbers from around the world, R,
1.6.2011,
http://www.reuters.com/article/2011/06/01/
us-aids-un-figures-idUSTRE75032920110601
"Mum sat next to me and said:
'You've got HIV'"
Despite the huge strides taken against Aids since the 1980s,
many young people with HIV still face stigma and shame
on a daily basis.
But in the New Year, the charity Body & Soul is launching
a campaign called In
My Shoes to raise awareness
in schools and youth clubs.
Here, some of those affected talk candidly
about living with HIV
– and why all
they want is a normal life
Sunday 5 December 2010
The Observer
Elizabeth Day
This article appeared on p34
of the Observer Magazine section of the Observer
on
Sunday 5 December 2010.
It was published on guardian.co.uk at 00.05 GMT
on Sunday 5 December 2010.
It was last modified at 09.49 GMT
on Monday 6 December 2010.
Peter is 22 years old and likes to look good. Today he is wearing
a dapper lime-green cardigan worn over a freshly pressed blue-and-white striped
polo-neck T-shirt. His glasses have thick black rims and rounded edges and
resemble something a rapper might wear in an ironic nod to the 1970s. "They're
from Specsavers," Peter says with a sheepish grin. "They have some good glasses
if you look hard enough."
But beneath the fashionable glasses and the easy smile, Peter has a secret. He
lives with this secret every day, the weight of it pressing down on him as soon
as he wakes up in the morning. He has not shared it with anyone outside his
immediate family or his most intimate circle of friends, and yet it is this
secret, perhaps more than anything else, that shapes the person he is, that
defines his life to such an extent that Peter cannot envisage what he would be
like if it did not exist.
Peter has HIV. It was transmitted to him from his mother, who sought asylum in
the UK after her home country in Africa descended into violent chaos. Peter was
three when he arrived in London. As a young child, he was prone to bouts of
illness and was in and out of hospital. At the age of 13, he spent three months
in a coma after a severe bout of meningitis. When he came round, the doctors
carried out some tests and discovered that his blood was infected with the human
immunodeficiency virus.
"I'd been getting loads of tests and stuff after the coma for my brain, but this
one day I remember we were taken to a different ward," he recalls. "Mum sat next
to me and said: 'I've got something to tell you. I don't know how you're going
to take this. You've got HIV.'"
He did not ask his mother how she contracted the virus – some things, he says,
are too hard to talk about, even with those closest to you. The diagnosis was
difficult to take in at first: Peter was told by his doctors that HIV gradually
destroys immune-system cells, reducing the body's protection against infection.
Over time, as the immune system weakens, someone affected by HIV may develop
rare infections or cancers. When these are especially serious, the person is
said to have acquired immune deficiency syndrome, or Aids. Despite the
substantial medical advances that have been made in recent years in managing the
disease, Peter was also informed that there is, as yet, no ultimate cure.
For Peter, the news came as a complete shock. He is one of six children and none
of his five brothers or sisters was infected. It felt, he says, like a death
sentence.
"I sat there, thinking: 'I'm 13 years old, what's the point of finishing
secondary school? I might as well save up and go travelling.' I just remember
thinking: 'Life is going to end quickly,' and that's what made me cry. The
thought that all my friends and stuff were going to live to old age and I'm just
going to fade away, they're going to forget me and how's my mum going to cope
without me? That's when I broke down. It was one of the worst days of my life.
It hurt so much." He breaks off, eyes focusing at a blank point in the middle of
the room. "Yeah, it hurt," he says finally, his voice small, the breath squeezed
out of it.
But then Peter was referred by the hospital to Body & Soul, a ground-breaking
charity supporting children, teenagers and families living with, or closely
affected by, HIV. The charity runs a purpose-built support centre in east
London, in a large, airy building filled with table-football games, computers
and coloured bean bags. It is one of the only organisations in the UK
specifically designed to help entire families, with a holistic approach that
provides youth groups, well-women clinics, yoga and therapy sessions as well as
information services providing welfare and benefits advice. Here, Peter can
socialise with other young people in exactly his situation.
Despite the extraordinary work Body & Soul does, it is not particularly high
profile as it is difficult to publicise – for obvious reasons, the people who
come here want their identities protected, which means it is harder for the
public to identify with their plight and put a face to the story. But in the New
Year, the charity will be launching a new campaign called In My Shoes to raise
awareness in schools and youth clubs, featuring portraits of celebrities and
teenagers affected by HIV, with their trainers obscuring their faces, taken by
the photographer Rankin.
"The idea is to try and get young people to understand what life is like from
other people's perspectives," explains Emma Colyer, the director of Body & Soul,
who co-founded the charity in 1996 after noticing there was almost no service
provision for women and children affected by HIV in the UK. "There's a lack of
understanding about HIV, and there's still a lot of stigma around the disease."
For Peter, Body & Soul gave him back his confidence. "After my diagnosis, I went
into a shell," he says. "I was shy and insecure about expressing myself again,
probably because of the shock, because I was scared of how people would react if
I was open with them.
"I remember the first day I came to Body & Soul. I heard I was going to a place
where people were infected with or affected by HIV. I expected to see people who
were sick, in wheelchairs. Instead, everyone was healthy and happy. I thought:
'I'm not in the right building.' Everyone seemed OK. Everyone gave you a hug.
They weren't afraid to touch you."
I was surprised to meet Peter, partly because he spoke so eloquently about his
status, with none of the recalcitrance or nervousness one might expect from a
young man in his early 20s. But if I am honest, it was also partly that I shared
the same misguided assumptions Peter had described all those years ago when he
first walked through the doors of Body & Soul: I had not expected someone living
with HIV to look so young or so healthy.
I grew up in the 1980s, at the time when the Aids epidemic was in its most
ferocious phase and the UK government posted leaflets to heighten the public's
awareness through the letterbox of every household in the country. Men and women
were dying at a frightening rate and there was intense media focus on the fact
that this rapidly spreading disease had no known cure. In 1987 an Australian
television advertisement for Aids awareness depicted the Grim Reaper mowing down
indiscriminate victims in a bowling alley. In the same year, the then chief
constable of Greater Manchester Police, James Anderton, claimed people were
"swirling around in a human cesspit of their own making" and people affected by
HIV were increasingly marginalised as authors of their own misfortune – the gay
men with promiscuous pasts or the drug users who passed round dirty needles.
Even as public perceptions began to shift – in 1987 the late Princess Diana did
much to tackle the social stigma of Aids patients by shaking their hands in
front of the television cameras – many of the cultural representations of people
living with HIV or Aids still centred on the idea of a middle-aged homosexual
man in the grip of a terrifying illness. When Tom Hanks won an Academy Award for
his portrayal of a lawyer dying from Aids in the 1993 movie Philadelphia, it was
for a performance that showed the central character as a gay man being horribly
ravaged by illness. In fact, only around 5-10% of HIV infection worldwide is as
a result of sex between men while two-thirds of people contract the virus
through heterosexual sex; in 2008 heterosexual sex accounted for 54% of HIV
diagnoses in the UK and sex between men accounted for 35%. But common
misconceptions still abound. Many of us do not expect people affected by HIV to
look like Peter: young, vibrant and healthy. We tend to forget that HIV has been
bequeathed to a new generation and that the virus now affects children,
teenagers and young adults alike – globally, Aids is the second most-common
cause of death among 20- to 24-year-olds and around 11% of HIV infections are
among babies who acquire the virus from their mothers.
It is a problem that continues to grow. According to the Health Protection
Agency, the rates of HIV infection in the UK are rising – an estimated 83,000
people who have HIV were living in the UK at the end of 2008, and more than a
quarter of them had been previously unaware of their status. One in every 500
people living in London has HIV. "When people think about HIV, they do think
about Africa," says Colyer. "They don't think about it here on our doorstep."
And although we might like to believe we are more educated about the virus now
than we were 30 years ago, substantial pockets of ignorance still remain. Last
year, a study of people who have HIV conducted by the People Living With HIV
Stigma Index found 21% of the 867 participants had been verbally abused or
harassed in the past 12 months because of their status. Twelve per cent had been
physically assaulted. Body & Soul recently commissioned a report on young
people's attitudes to HIV from the Office for Public Management. The
questionnaire, of more than 500 12- to 18-year-olds, found that despite
increased awareness of the facts, there was a contradiction between their
knowledge and their behaviour. So although 81% of respondents knew the virus
could not be transmitted by sharing a cup, only 27% of them said they would
actually be willing to drink from the same cup as a person they knew was HIV
positive. Eleven per cent said they would not remain friends with someone who
has HIV.
The report goes on to state that the respondents "appeared to distance
themselves mentally from people living with HIV through a process of 'othering'
them: imagining they are very different from themselves. In particular, that
they either live in developing countries and are therefore far away, or have got
HIV through 'bad' lifestyle choices – doing things which they'd never choose to
do themselves."
It is a statement backed up again and again by the experiences of those I speak
to at Body & Soul. Michelle, a pretty and vivacious 23-year-old, was dumped by
her boyfriend of four years after she told him she had HIV. "He went through an
angry phase. I found out he was cheating on me, and when I challenged him, he'd
throw things at me, like saying: 'It's not as if I'm going to bring back any
diseases. You've got that already.' After we split up, he sent me text messages
like: 'You're going to die. How can you live with that disease? You'll never get
a relationship with anyone else.'"
Michelle clutches her mug of coffee more closely to her chest as she talks. Her
fingernails are exquisitely painted, each one emblazoned with a tiny picture of
a palm tree rendered in multicoloured polish. In fact her HIV was not a
consequence of those supposedly "bad" lifestyle choices, but an unlucky accident
of birth – Michelle was born in a developing country in Africa, and at some
point the doctors looking after her infected her with the virus, probably by
using an unsterilised needle. "I went through a lot of stages before I accepted
it," Michelle says. "For a long time, I kind of pretended it wasn't real.
Sometimes, with a lot of us, I feel we're living double lives because we can't
tell anyone about our HIV."
Peter, too, has had his share of uncomfortable experiences. He once told a
friend at university, only to discover several months later that the friend had
been talking about him behind his back. "He was saying: 'I need to start washing
my plates. I need to get tested.'" Did that make Peter upset? "It didn't anger
me; it just made me understand that a lot of people are still ignorant. We still
need to educate people so that when someone else comes out and says: 'I've got
HIV,' they won't step back, but come forward." Interestingly, Peter says he has
never faced overt racism while living in the UK: for him, the stigma attached to
HIV is far more pervasive and difficult to tackle.
There are other stories, too, of a four-year-old child with the virus being
asked to leave school, of a 14-year-old girl being bullied by her classmates
because of her status, of a woman who told her dentist she was HIV positive and
was then refused treatment. There are families who reject their own flesh and
blood – one young woman's parents died when she was little, but because she had
HIV, her relatives would not take her in: they took her brother instead and she
ended up in foster care.
It is for this reason that Body & Soul performs such a crucial function,
enabling people like Peter and Michelle to talk freely about their lives and to
socialise in an environment where they will not be judged. Every week, around
250 people, ranging in age from newborn babies to adults in their 40s, drop in
to the charity's headquarters. Sometimes several members of the same family come
at once, whether they have HIV themselves or are affected by living with a
relative who has the virus.
A team of 14 staff members and 150 volunteers puts on a range of weekly
activities for different age groups. The youngest children are entertained in an
Ofsted-accredited nursery filled with toys, while teenagers can make use of a
state-of-the-art recording studio in the basement. Adults are offered
creative-writing classes or the chance to take part in group debates. One-to-one
counselling is readily available, and there are also massage and therapy rooms.
Regular hot meals are provided, as well as taxis to and from the venue for those
who are too ill to use public transport.
Although HIV is now considered a "chronic, manageable disease" by some health
experts because of advances in antiretroviral drugs, these often come with
unpleasant side-effects and some people build up resistance to certain drugs, so
much of the treatment can be an exhausting exercise in trial and error.
Often a teenager who has HIV, who is desperate to live as normal a life as
possible, will rebel against the disease by refusing to take their medication.
When Michelle was given her first batch of tablets to swallow four years ago,
she says, "I didn't like the taste. I didn't feel I needed them and I refused to
take them. I was in denial. But then I got really ill and I had to come to terms
with everything. It was hard to accept that I would be living my life so
differently."
In April Michelle's best friend died after he failed to take his medicines. "He
just wanted to live a normal life," she says. "He was 23, same age as me. We
were so close he used to call me his cousin. He hid away a lot before he died;
he didn't want to see anybody. He's kind of my inspiration now. I can't go down
that road [of not taking medicines]. If not for me, then for him."
And sometimes it is easy to forget, talking to the bright and engaging people I
meet at Body & Soul, that many of them have had to deal with extreme pain,
isolation and trauma. These are people who are unwilling to be portrayed as
victims and yet who have survived such brutality that sometimes the only
response is to cry.
These are people like Victoria, a 42-year-old mother of four. She sits neatly in
a chair with her hands on her lap as she talks, wearing a red polo neck and a
duffle coat matched to precisely the same shade. Her hair is plaited, swept up
in a high ponytail held in place with a polka-dotted hairpin. She tells me she
grew up in a country in central Africa but was forced to seek asylum in Britain
when it slid into civil war. In 2003 she left behind her husband, her parents
and her two eldest sons. She was seven months pregnant at the time.
Victoria spent several weeks in detention before being relocated to a market
town in the northeast of England, a place where she knew no one. It was only
when the doctors started treating her for tuberculosis that she discovered she
also had HIV. For several months after Victoria was diagnosed, she slid into an
abyss of depression. "I would close the door and the window and I would wait to
die." Eventually she moved to London, where she was told about Body & Soul.
Victoria believes she contracted the virus after she was raped at the age of 22.
She had taken the bus to visit her boyfriend in a village four hours from her
own. When she got off the bus, it was already dark. She started walking and
noticed a shape coming out of nowhere, emerging then disappearing. "Somebody
grabbed me," Victoria remembers. "I tried to shout, but he beat me up. He beat
me and then he raped me. And after he raped me I ran to the village and people
asked me had anything happened to me and I said: 'No' because I was scared. I
did not even tell my boyfriend." The tears start to roll down her cheeks. She
sobs quietly, her breaths ragged. "It never goes away. I think about it day and
night because now my seven-year-old son has HIV, too, and it is a burden. I feel
very, very guilty because whenever I go to pick him up from school, he's there
looking pale and tired and his teachers ask: 'Why does he never smile?'"
If it were not for Body & Soul, Victoria says she would not have been able to
cope. She comes every Tuesday for counselling while her son, who has behavioural
problems, has "play therapy". "Sometimes you come when you're really down and
you just want to talk. I've made a really good friend here. I call her whenever
I'm stuck and she gives me so much advice. I think Body & Soul is the only place
I feel confident. In the outside world I feel that other people are reading me,
like they know who I am. I feel different, I feel bad. But here I can be
myself." Victoria smiles briefly, and then looks me straight in the eye. "I tell
you," she says, nodding her head to mark the gravity of every single word, "it
saved my life."
We finish talking and Victoria gets up from her seat, wrapping her coat tightly
around her as though for protection. I imagine her walking through the
drizzle-dampened city streets outside, arms crossed in front of her chest,
people pushing and jostling past her on their way home. I imagine the weight of
the secret she carries within her, the pressure of knowing it will always be
there. And I am glad that she has this shelter to return to – a place where she
can be herself, where she can take off her coat and let the warmth seep through
her.
Elizabeth Day is a feature writer at the Observer.
Her debut
novel, Scissors, Paper, Stone,
is published by Bloomsbury in January.
"Mum sat next to me and
said: 'You've got HIV'", O, 5.12.2010,
http://www.guardian.co.uk/society/2010/dec/05/hiv-aids-body-and-soul
Daily Pill Lowers H.I.V. Infection Risk,
Study Finds
November 23, 2010
The New york Times
By DONALD G. McNEIL Jr.
In a development that could change the battle against AIDS, researchers have
found that taking a daily antiretroviral pill greatly lowers the chances of
getting infected with the virus.
In the study, published Tuesday by the New England Journal of Medicine,
researchers found that the hundreds of gay men randomly assigned to take the
drugs were 44 percent less likely to get infected than the equal number assigned
to take a placebo.
But when only the men whose blood tests showed they had taken their pill
faithfully every day were considered, the pill was more than 90 percent
effective, said Dr. Anthony S. Fauci, head of the division of the National
Institutes of Health, which paid for the study along with the Bill and Melinda
Gates Foundation.
“That’s huge,” Dr. Fauci said. “That says it all for me.”
The large study, nicknamed iPrEx, included nearly 2,500 men in six countries and
was coordinated by the Gladstone Institutes of the University of California, San
Francisco.
The results are the best news in the AIDS field in years, even better than this
summer’s revelation that a vaginal microbicide protected 39 percent of all the
women testing it and 54 percent of those who used it faithfully.
Also, the antiretroviral pill — Truvada, a combination of two drugs, tenofovir
and emtricitabine — is available by prescription in many countries right now,
while the microbicide gel is made only in small amounts for clinical trials.
The protection, known as “pre-exposure prophylaxis” or “PreP,” is also the first
new form available to men, especially men who cannot use condoms because they
sell sex, are in danger of prison rape, are under pressure from partners or lose
their inhibitions when drunk or high.
It is a form of protection “that does not involve getting permission from the
other partner, and that’s important,” said Phill Wilson, president of the Black
AIDS Institute, which focuses on the epidemic among blacks.
Michel Sidibé, the head of UNAIDS, the United Nations AIDS-fighting agency,
called it “a breakthrough that will accelerate the prevention revolution.”
Because Truvada is available now, some clinicians already prescribe it for
prophylaxis, Dr. Fauci said, but whether doing so becomes official policy will
depend on discussions by the Centers for Disease Control and Prevention, the
Food and Drug Administration, medical societies and others, which could take
months.
Although the C.D.C. would prefer that doctors wait for further studies, more
probably will prescribe it now that this study is out, said Dr. Kevin Fenton,
chief of the agency’s AIDS division, so the C.D.C. will soon release suggested
guidelines.
The agency will encourage that the drug be prescribed only with close medical
supervision and used only with other safe-sex practices, treatment for venereal
diseases and counseling.
“The results are encouraging, but it’s not time for gay men to throw away their
condoms,” Dr. Fenton said.
AIDS advocacy groups were very excited by the results.
“If you comply with it, this works really well,” said Chris Collins, policy
director of amfAR, the Foundation for AIDS Research. “This is too big to walk
away from.”
Mitchell Warren, executive director of AVAC, which lobbies for AIDS prevention,
called the study “a great day for the fight against AIDS” and said gay men and
others at risk needed to be consulted on the next steps.
AIDS experts and the researchers issued several caveats about the study’s
limitations.
It was only of gay men and only of one drug combination. More studies, now under
way, are needed to see if they duplicate these results and to see whether
Truvada also protects heterosexual men and women, prostitutes and drug users who
share needles, and whether other drugs will work, too.
There is no medical reason to think the pill would not work in everyone, since
it attacks the virus in the blood, rather than in the vaginal wall as a
microbicide does.
Different regimens, like taking the pills only when sex is anticipated instead
of daily, also need testing.
Also, many men in the study failed to take all their pills, and some clearly
lied about it. For example, some who claimed to take them 90 percent of the time
had little or no drug in their bloodstreams.
Although the pills caused no major side effects in the study, some men disliked
the relatively minor ones, like nausea and headaches. Also, as is common in
clinical trials, some stopped bothering once they suspected they might be taking
a placebo.
“People have their own reasons,” Mr. Collins said. “People don’t take their
Lipitor every day either.”
A major question now is who will pay for the drug.
In the United States, Truvada, made by Gilead Sciences, costs $12,000 to $14,000
a year. In very poor countries, generic versions costs as little as 40 cents a
pill.
Globally, only about 5 million of the 33 million people with AIDS are on
antiretrovirals, and, in an era of tight foreign-aid budgets, that number is not
expected to rise quickly.
Hundreds of millions of Africans, eastern Europeans and Asians are at risk and
could benefit from prophylaxis, but that would cost tens of billions of dollars.
If he had the money, Mr. Sidibé of UNAIDS said, he would target high-risk groups
like sex workers, gay men, drug users and uninfected people married to infected
people.
In this country, insurers and Medicare normally pay for the drugs, and the Ryan
White Act covers the cost for the poor — but none of these payers yet have
policies on supplying the drugs to healthy people.
One fear some scientists have is that putting more people on the drugs will
speed the evolution of drug-resistant strains.
None of the 2,499 participants developed resistance to tenofovir. Three were
found to have strains resistant to emtricitabine, but investigators believe all
three were infected before the study began, but at levels low enough to have
been missed by their first H.I.V. tests.
Because participants were tested monthly and those who got infected were put on
triple therapy cocktails, it was unlikely any were on two-drug Truvada long
enough to develop drug resistant strains.
Another fear was that the participants would become so fearless that they would
stop using condoms, but the opposite effect was seen — they used condoms more
often and had fewer sex partners. But that can also be a function of simply
being enrolled in a study and getting a steady diet of safe sex advice and free
condoms, the investigators said.
The study took place at 11 sites in the United States, South Africa, Brazil,
Thailand, Ecuador and Peru. Other trials of pre-exposure prophylaxis have about
20,000 volunteers enrolled around the world. Their results are expected to
arrive in a steady stream over the next two years.
Daily Pill Lowers H.I.V.
Infection Risk, Study Finds, 23.11.2010,
http://www.nytimes.com/2010/11/24/health/research/24aids.html
Precursor to H.I.V.
Was in Monkeys for Millennia
September 16, 2010
The New York Times
By DONALD G. McNEIL Jr.
In a discovery that sheds new light on the history of AIDS,
scientists have found evidence that the ancestor to the virus that causes the
disease has been in monkeys and apes for at least 32,000 years — not just a few
hundred years, as had been previously thought.
That means humans have presumably been exposed many times to S.I.V., the simian
immunodeficiency virus, because people have been hunting monkeys for
millenniums, risking infection every time they butcher one for food.
And that assumption in turn complicates a question that has bedeviled AIDS
scientists for years: What happened in Africa in the early 20th century that let
a mild monkey disease move into humans, mutate to become highly transmissible
and then explode into one of history’s great killers, one that has claimed 25
million lives so far?
Among the theories different researchers have put forward are the growth of
African cities and the proliferation of cheap syringes.
Confirming that the virus is very old also helps explain why it infects almost
all African monkeys but does not sicken them. Over many generations, as any
disease kills off vulnerable victims, the host adapts to it.
The new research, published Thursday in Science magazine, was relatively simple.
Scientists tested 79 monkeys from Bioko, a volcanic island 19 miles off the West
African coast. Bioko used to be the end of a peninsula attached to the mainland
in what is now Cameroon, but it was cut off when sea levels rose 10,000 years
ago at the end of the last ice age.
Since then, six monkey species have developed in isolation on the island, and
scientists from the National Primate Research Center at Tulane University in
Louisiana and other American and African universities found that four of them —
drills, red-eared guenons, Preuss’s guenons and black colobuses — had members
that were infected with S.I.V.
The four strains in the four species were genetically very different from one
another — meaning they presumably did not come from monkeys carried over to the
island by humans in the last few centuries. But each was close to the strain
infecting members of the same four genuses on the mainland, meaning they must
have existed before Bioko was cut off.
Knowing that all four strains were at least 10,000 years old, scientists
recalculated the virus’s “molecular clock,” measuring how fast it mutates. They
now believe that all the S.I.V. strains infecting monkeys and apes across Africa
diverged from a common ancestor between 32,000 and 78,000 years ago.
“When we only had 25 years of data, we were dating from the tip at the end of a
branch of the evolutionary tree,” said Preston A. Marx, a virologist at the
Tulane primate center and an author of the paper in Science. “I knew that what
we had before couldn’t be right, because the virus had spread from the Atlantic
to the Indian Ocean to the southern end of the continent, and it couldn’t have
done that in a couple of hundred years.”
Beatrice H. Hahn, a virologist from the University of Alabama at Birmingham and
a discoverer of the simian virus, called the study “a very nice paper,” adding,
“This is what people like us have been looking for.”
Previous methods of dating the virus had concluded it was a few hundred to 2,000
years old, “and that just didn’t seem right,” Dr. Hahn said.
The ancestor virus — which, like many diseases, may have crossed into simians
from another, still-unknown species — may have existed for millions of years.
That theory was given greater credence two years ago with the discovery that
some Madagascar lemurs have in their genomes the remnants of a virus that was
not an S.I.V., but related to it. Madagascar, a Texas-size island 250 miles off
the southeastern African coast, separated from Africa 160 million years ago. It
has no monkeys, but lemurs’ ancestors arrived there, possibly on floating mats
of vegetation, probably more than 10 million years ago.
H.I.V., which is almost universally fatal to humans, is obviously very new to
us. As Dr. Marx pointed out, if it had been in humans before the 20th century,
it would have arrived in the Americas in some of the 12 million Africans
kidnapped for the slave trade.
Its immediate ancestor is probably also relatively new to chimpanzees. Last
year, Dr. Hahn showed that it can sicken and kill chimps, although not as
quickly, meaning they have probably been adapting to it for generations.
The virus has probably crossed over from simians into humans at least five
times. There are two human immunodeficiency viruses, H.I.V.-1, by far the most
common, and H.I.V.-2, which is milder and rarely seen outside West Africa, and
which jumped to humans from sooty mangabeys, a monkey that West Africans hunt
and eat.
H.I.V.-1, in turn, has four substrains, designated M, N, O and P. The first,
which has spread around the world, clearly came from chimpanzees, as did N and
O. But P appears to have crossed over from a gorilla; it was discovered only
last year, and in only one woman, who was from Cameroon, where lowland gorillas
are hunted for meat.
It is very likely, scientists said, that a little infected monkey or ape blood
got into human veins many times in history as hunters cut themselves while
butchering carcasses. But even if it sickened those hunters, it probably died
out with them or their immediate contacts.
The earliest confirmed H.I.V. case in humans was found in blood drawn in 1959
from a man in Kinshasa, in what was then called the Belgian Congo.
Sometime between the 1800s and 1959, something presumably allowed a human
infection with a chimpanzee virus to spread widely enough to evolve into modern
H.I.V.-1, which could spread easily among humans.
Dr. Marx believes that the crucial event was the introduction into Africa of
millions of inexpensive, mass-produced syringes in the 1950s. Campaigns to wipe
out yaws, syphilis, malaria, smallpox and polio required syringes, and many were
reused, often with official approval. Traditional healers adopted them for
injecting their decoctions, and they became status symbols; a study in Uganda in
the 1960s found that 80 percent of families owned one.
Not everyone agrees. Michael Worobey, a virologist at the University of Arizona
and another author of the Science paper, said backdating the molecular clock,
which he did by comparing the 1959 blood sample with the only other known early
one — a paraffin-embedded lymph node from 1960, also from Kinshasa — suggested
that the virus emerged closer to 1910, when syringes were handmade, expensive
and rare.
He and Dr. Hahn suspect that the growth of colonial cities is to blame. Before
1910, no Central African town had more than 10,000 people. But urban migration
rose, increasing sexual contacts and leading to red-light districts.
Precursor to H.I.V. Was
in Monkeys for Millennia, NYT, 16.9.2010,
http://www.nytimes.com/2010/09/17/health/17aids.html
Obama to Outline Plan
to Cut H.I.V. Infections
July 11, 2010
The New York Times
By ROBERT PEAR
WASHINGTON — President Obama will unveil a new national strategy this week to
curb the AIDS epidemic by slashing the number of new infections and increasing
the number of people who get care and treatment.
“Annual AIDS deaths have declined, but the number of new infections has been
static and the number of people living with H.I.V. is growing,” says a final
draft of the report, obtained by The New York Times.
In the report, the administration calls for steps to reduce the annual number of
new H.I.V. infections by 25 percent within five years. “Approximately 56,000
people become infected each year, and more than 1.1 million Americans are living
with H.I.V.,” the report says.
Mr. Obama plans to announce the strategy, distilled from 15 months of work and
discussions with thousands of people around the country, at the White House on
Tuesday.
While acknowledging that “increased investments in certain key areas are
warranted,” the report does not propose a major increase in federal spending. It
says the administration will redirect money to areas with the greatest need and
population groups at greatest risk, including gay and bisexual men and
African-Americans. The federal government now spends more than $19 billion a
year on domestic AIDS programs.
On average, the report says, one person is newly infected with H.I.V. every nine
and a half minutes, but tens of thousands of people with the virus are not
receiving any care. If they got care, the report says, they could prolong their
own lives and reduce the spread of the virus to others. By 2015 the report says,
the United States should “increase the proportion of newly diagnosed patients
linked to clinical care within three months of their H.I.V. diagnosis to 85
percent,” from the current 65 percent.
The first-ever national AIDS strategy has been in the works since the start of
the administration. It comes in the context of growing frustrations expressed by
some gay rights groups. They say that more money is urgently needed for the AIDS
Drug Assistance Program, and they assert that the White House has not done
enough to secure repeal of the law banning military service by people who are
openly gay or bisexual.
The report tries to revive the sense of urgency that gripped the nation in the
first years after discovery of the virus that causes AIDS. “Public attention to
the H.I.V. epidemic has waned,” the report says. “Because H.I.V. is treatable,
many people now think that it is no longer a public health emergency.”
The report calls for “a more coordinated national response to the H.I.V.
epidemic” and lays out specific steps to be taken by various federal agencies.
Mr. Obama offers a compliment to President George W. Bush, who made progress
against AIDS in Africa by setting clear goals and holding people accountable.
The program begun by Mr. Bush, the President’s Emergency Plan for AIDS Relief,
“has taught us valuable lessons about fighting H.I.V. and scaling up efforts
around the world that can be applied to the domestic epidemic,” the report says.
Mr. Obama’s strategy is generally consistent with policies recommended by public
health specialists and advocates for people with H.I.V. But some experts had
called for higher goals, more aggressive timetables and more spending on
prevention and treatment.
The report makes these points:
¶Far too many people infected with H.I.V. are unaware of their status and may
unknowingly transmit the virus to their partners. By 2015, the proportion of
people with H.I.V. who know of their condition should be increased to 90
percent, from 79 percent today.
¶The new health care law will significantly expand access to care for people
with H.I.V., but federal efforts like the Ryan White program will still be
needed to fill gaps in services.
¶Federal spending on H.I.V. testing and prevention does not match the need.
States with the lowest numbers of H.I.V./AIDS cases often receive the most money
per case. The federal government should allocate more of the money to states
with the highest “burden of disease.”
¶Health officials must devote “more attention and resources” to gay and bisexual
men, who account for slightly more than half of new infections each year, and
African-Americans, who account for 46 percent of people living with H.I.V.
¶The H.I.V. transmission rate, which indicates how fast the epidemic is
spreading, should be reduced by 30 percent in five years. At the current rate,
about 5 of every 100 people with H.I.V. transmit the virus to someone in a given
year.
If the transmission rate is unchanged, the report says, “within a decade, the
number of new infections would increase to more than 75,000 per year and the
number of people living with H.I.V. would grow to more than 1.5 million.”
The report finds that persistent discrimination against people with H.I.V. is a
major barrier to progress in fighting the disease.
“The stigma associated with H.I.V. remains extremely high,” it says. “People
living with H.I.V. may still face discrimination in many areas of life,
including employment, housing, provision of health care services and access to
public accommodations.”
The administration promises to “strengthen enforcement of civil rights laws”
protecting people with H.I.V.
One political challenge for the administration is to win broad public support
for a campaign that will focus more narrowly on specific groups and communities
at high risk for H.I.V. infection.
“Just as we mobilize the country to support cancer research whether or not we
believe that we are at high risk of cancer and we support public education
whether or not we have children,” the report says, “fighting H.I.V. requires
widespread public support to sustain a long-term effort.”
Obama to Outline Plan to
Cut H.I.V. Infections, NYT, 11.7.2010,
http://www.nytimes.com/2010/07/12/health/policy/12aids.html
The Wavering War on AIDS
May 13, 2010
The New York Times
The global war on AIDS has racked up enormous successes over the past decade,
most notably by providing drugs for millions of infected people in developing
countries who would be doomed without this life-prolonging treatment. Now the
campaign is faltering.
Donations from the United States and other wealthy countries have leveled off
while the number of people infected with H.I.V., the AIDS virus, grows by a
million a year. By one informed estimate, only $14 billion will be available of
some $27 billion needed this year to fight the disease in the developing world.
Fewer than 4 million of the 14 million people infected with the AIDS virus are
getting drug treatment — far short of the goal of universal access set by the
United States and others.
Donor nations cite the economic crisis and tight budgets as reasons to slow
their contributions to the global fight against AIDS. The Obama administration
and many donor nations apparently believe that more lives could be saved by
fighting other cheaper diseases, such as respiratory illnesses, diarrhea,
malaria and measles.
The results of those decisions can be seen in Uganda and other countries where,
as Donald G. McNeil Jr. recently reported in The Times, the campaign against
AIDS seems to be falling apart.
Although the number of Ugandans receiving drug treatments jumped from fewer than
10,000 a decade ago to nearly 200,000 today, hundreds of thousands more Ugandans
need the drugs and likely can’t get them because clinics now routinely turn new
patients away.
That is partly because American funds have been frozen and clinics were told to
stop enrolling new patients unless the government has a plan to pay for their
treatment. It is also because Uganda has badly skewed its own priorities, such
as negotiating to buy a squadron of fighter-bombers from Russia for $300
million.
The United States has been a leader in providing financing for the war on AIDS
through bilateral programs and a multilateral global fund. Now, instead of a
sharp increase in donations, as once planned, the administration proposes only a
slight increase in bilateral financing and a modest reduction in its
multilateral contribution.
It has shifted its focus to childhood diseases, keeping young mothers alive, and
interrupting the transmission of H.I.V. between mother and child. It is pushing
countries to improve their medical delivery systems, manage their own AIDS
programs and contribute more of their own funds.
Those are good goals. But the AIDS pandemic is still spreading. And the goal of
universal access to treatment remains a distant dream.
The Wavering War on
AIDS, NYT, 31.5.2010,
http://www.nytimes.com/2010/05/14/opinion/14fri2.html
After Long Scientific Search,
Still No Cure for AIDS
May 9, 2010
The New York Times
By DONALD G. McNEIL Jr.
Despite decades of effort, no magic bullet for AIDS has been invented.
The obstacles are huge. The virus mutates as fast in a day as a flu virus does
in a year, but can also lie dormant indefinitely.
Since no one has ever been cured, there is no natural defense to mimic. And,
since it attacks the CD4 cells that are the “fire alarms” of the immune system,
vaccines that stimulate immunity may just give it more targets.
Even in wealthy countries, it can only be controlled; antiretroviral cocktails
keep it from replicating. Patients are not cured, but may survive into old age.
With just four million people on treatment worldwide and donors balking at the
idea of supporting 33 million or more, a miracle is needed. But none is on the
horizon.
The latest failed vaccine trial, in Thailand, took six years. It may have
temporarily protected a few participants, but even that required six shots
spaced months apart. That is too complicated for places like rural Africa, where
polio drives often fail, though they involve only a few pink drops in babies’
mouths. Dr. Anthony S. Fauci, who oversaw the Thai trial, said he saw “no
chance” of a vaccine in the next few years and a “reasonable” chance of one in
20 years.
The quest for a vaginal microbicide is also stalled. Women need a product that
is not messy and can be inserted secretly, because many men react furiously to
any suggestion that they are infected.
Also, because many women want children, it must block a tiny virus without
blocking sperm, which has been likened to stopping a million BBs streaming down
a road while a fleet of Mack trucks breezes through.
Trials using sticky chemicals have proved futile. An early trial of a spermicide
actually increased infections.
In July, results are due from a trial of a gel containing the antiretroviral
drug tenofovir, which worked well in monkeys. It is expected to show neither a
major breakthrough nor an utter failure, since, ethically, scientists would have
had to stop the trial prematurely if preliminary results showed either trend.
Sharon Hillier, principal investigator for the Microbicide Trials Network, said
she was still “hopeful” that such a gel, or a vaginal implant that released
drugs slowly, would be ready some day.
“But,” Dr. Hillier said, “it’s going to be a long and difficult passage.”
After Long Scientific
Search, Still No Cure for AIDS, NYT, 9.5.2010,
http://www.nytimes.com/2010/05/10/world/africa/10aidsscience.html
Study
Cites Toll of AIDS Policy
in South Africa
November
26, 2008
The New York Times
By CELIA W. DUGGER
JOHANNESBURG — A new study by Harvard researchers estimates that the South
African government would have prevented the premature deaths of 365,000 people
earlier this decade if it had provided antiretroviral drugs to AIDS patients and
widely administered drugs to help prevent pregnant women from infecting their
babies.
The Harvard study concluded that the policies grew out of President Thabo
Mbeki’s denial of the well-established scientific consensus about the viral
cause of AIDS and the essential role of antiretroviral drugs in treating it.
Coming in the wake of Mr. Mbeki’s ouster in September after a power struggle in
his party, the African National Congress, the report has reignited questions
about why Mr. Mbeki, a man of great acumen, was so influenced by AIDS
denialists.
And it has again caused soul-searching about why his colleagues in the party did
not act earlier to challenge his resistance to broadly accepted methods of
treating and preventing AIDS.
Reckoning with a legacy of such policies, Mr. Mbeki’s’s successor, Kgalema
Motlanthe, acted on the first day of his presidency two months ago to remove the
health minister, Manto Tshabalala-Msimang, a polarizing figure who had proposed
garlic, lemon juice and beetroot as AIDS remedies.
He replaced her with Barbara Hogan, who has brought South Africa — the most
powerful country in a region at the epicenter of the world’s AIDS pandemic —
back into the mainstream.
“I feel ashamed that we have to own up to what Harvard is saying,” Ms. Hogan, an
A.N.C. stalwart who was imprisoned for a decade during the anti-apartheid
struggle, said in a recent interview. “The era of denialism is over completely
in South Africa.”
For years, the South African government did not provide antiretroviral
medicines, even as Botswana and Namibia, neighboring countries with epidemics of
similar scale, took action, the Harvard study reported.
The Harvard researchers quantified the human cost of that inaction by comparing
the number of people who got antiretrovirals in South Africa from 2000 to 2005
with the number the government could have reached had it put in place a workable
treatment and prevention program.
They estimated that by 2005, South Africa could have been helping half those in
need but had reached only 23 percent. By comparison, Botswana was already
providing treatment to 85 percent of those in need, and Namibia to 71 percent.
The 330,000 South Africans who died for lack of treatment and the 35,000 babies
who perished because they were infected with H.I.V. together lost at least 3.8
million years of life, the study concluded.
Epidemiologists and biostatisticians who reviewed the study for The New York
Times said the researchers had based their estimates on conservative assumptions
and used a sound methodology.
“They have truly used conservative estimates for their calculations, and I would
consider their numbers quite reasonable,” James Chin, a professor of
epidemiology at the University of California at Berkeley’s School of Public
Health, said in an e-mail message.
The report was posted online last month and will be published on Monday in the
peer-reviewed Journal of Acquired Immune Deficiency Syndromes.
Max Essex, the virologist who has led the Harvard School of Public Health’s AIDS
research program for the past 20 years and who oversaw the study, called South
Africa’s response to AIDS under Mr. Mbeki “a case of bad, or even evil, public
health.”
Mr. Mbeki has maintained a silence on his AIDS legacy since his forced
resignation. His spokesman, Mukoni Ratshitanga, said Mr. Mbeki would not discuss
his thinking on H.I.V. and AIDS, explaining that policy decisions were made
collectively by the cabinet and so questions should be addressed to the
government.
The new government is now trying to hasten the expansion of antiretroviral
treatments. The task is urgent. South Africa today is home to 5.7 million people
who are H.I.V.-positive — more than any other nation, almost one in five adults.
More than 900 people a day die here as a result of AIDS, the United Nations
estimates.
Since the party forced Mr. Mbeki from office and some of his loyalists split off
to start a new party, rivalries have flared and stories about what happened
inside the A.N.C. have begun to tumble out, offering unsettling glimpses of how
South Africa’s AIDS policies went so wrong.
From the first year of his presidency in 1999, Mr. Mbeki became consumed with
the thinking of a small group of dissident scientists who argued that H.I.V. was
not the cause of AIDS, his biographers say.
As president he wielded enormous power, and those who disagreed with him said
they feared they would be sidelined if they spoke out. Even Nelson Mandela, the
revered former president, was not immune from opprobrium.
In a column in The Sunday Times of Johannesburg on Oct. 19, Ngoako Ramatlhodi, a
senior party member now running the party’s 2009 election campaign, recounted
how Mr. Mandela, known affectionately as Madiba, was humiliated during a 2002
A.N.C. meeting after he made a rare appearance to question the party’s stance on
AIDS.
Mr. Ramatlhodi described speakers competing to show greater loyalty to Mr. Mbeki
by verbally attacking Mr. Mandela as Mr. Mbeki looked on silently. “After his
vicious mauling, Madiba looked twice his age, old and ashen,” Mr. Ramatlhodi
wrote.
Mr. Ramatlhodi himself acknowledged in a recent interview that in 2001 he sent a
22-page letter, drafted by Mr. Mbeki’s office, to another of Mr. Mbeki’s most
credible critics, Prof. Malegapuru Makgoba, an immunologist who was one of South
Africa’s leading scientists. The letter accused Professor Makgoba of defending
Western science and its racist ideas about Africans at the expense of Mr. Mbeki.
In 2000 Mr. Mbeki had provided Professor Makgoba with two bound volumes
containing 1,500 pages of documents written by AIDS denialists. After reading
them, Professor Makgoba said in an interview that he wrote back to warn Mr.
Mbeki that if he adopted the denialists’ ideas, South Africa would “become the
laughingstock, if not the pariah, of the world again.”
But Mr. Mbeki indicated last year to one of his biographers, Mark Gevisser, that
his views on AIDS were essentially unchanged, pointing the writer to a document
that, he said, was drafted by A.N.C. leaders and accurately reflected his
position.
The document’s authors conceded that H.I.V. might be one cause of AIDS but
contended that there were many others, like other diseases and malnutrition.
The document maintained that antiretrovirals were toxic. And it suggested that
powerful vested interests — drug companies, governments, scientists — pushed the
consensus view of AIDS in a quest for money and power, while peddling
centuries-old white racist beliefs that depicted Africans as sexually rapacious.
“Yes, we are sex crazy!” the document’s authors bitterly exclaimed. “Yes, we are
diseased! Yes, we spread the deadly H.I. virus through our uncontrolled
heterosexual sex!”
In 2002, after a prolonged outcry over Mr. Mbeki’s comments about AIDS and the
government’s policies, Mr. Mbeki agreed to requests from within his party to
withdraw from the public debate. That same year, the Constitutional Court ruled
that the government had to provide antiretroviral drugs to prevent the infection
of newborns. And in 2003, the cabinet announced plans to go forward with an
antiretroviral treatment program.
“We did an enormous amount of good in the early days in South Africa, not
because of the Health Ministry, but in spite of the Health Ministry,” said
Randall L. Tobias, who was appointed by President Bush in 2003 to lead the
United States’ $15 billion global AIDS undertaking.
In the same years, former President Clinton and his foundation were also deeply
involved in helping South Africa get a treatment program going. Mr. Clinton
attended Mr. Mandela’s 85th birthday celebration in Johannesburg in 2003. During
the dinner, he and Mr. Mbeki slipped away to talk about AIDS, Mr. Clinton
recalled in a recent interview.
Mr. Clinton said he told Mr. Mbeki how antiretroviral treatment had reduced the
AIDS mortality rate in the United States and reminded him, “I’m your friend and
I haven’t joined in the public condemnation.” That evening, when Mr. Clinton
offered to send in a team of experts to help the country put together a national
treatment plan, Mr. Mbeki took him up on it.
The Clinton Foundation helped devise a plan and mobilized 20 people to travel to
South Africa in 2004 to help carry it out. But the South African government
never invited them, Mr. Clinton said. So the foundation, which had projects all
over Africa, was to have none in South Africa.
Changes since Mr. Mbeki’s fall from power have prompted many to hope for
forceful South African political leadership on AIDS. Mr. Mbeki’s rival and
successor as head of the party, Jacob Zuma, who is expected to become president
after next year’s election, himself made a famously questionable remark about
AIDS.
In his 2006 rape trial, in which he was acquitted of sexually assaulting a
family friend, he testified that he sought to reduce his chances of being
infected with H.I.V. by taking a shower after sex. Nonetheless, he seems to have
more conventional views on the pandemic.
“Who would have thought Jacob Zuma would be better than Mbeki, but he is,” said
Richard C. Holbrooke, the former ambassador to the United Nations in the Clinton
administration who heads a coalition of businesses fighting AIDS. “The tragedy
of Thabo Mbeki is that he’s a smart man who could have been an international
statesman on this issue. To this day, you wonder what got into him.”
For South Africans who watched the dying and were powerless to stop it, the
grief is still raw. Zackie Achmat, the country’s most prominent advocate for
people with AIDS, became sick during the almost five years he refused to take
antiretrovirals until they were made widely available. He cast Mr. Mbeki as the
leading man in this African tragedy.
“He is like Macbeth,” Mr. Achmat said. “It’s easier to walk through the blood
than to turn back and admit you made a mistake.”
Study Cites Toll of AIDS Policy in South Africa, NYT,
26.11.2008,
http://www.nytimes.com/2008/11/26/world/africa/26aids.html
H.I.V.
Is Spreading in New York City
at Three Times the National Rate,
a Study Finds
August 28,
2008
The New York Times
By SEWELL CHAN
The virus
that causes AIDS is spreading in New York City at three times the national rate
— an incidence of 72 new infections for every 100,000 people, compared with 23
per 100,000 nationally — according to a study released on Wednesday by the
city’s Department of Health and Mental Hygiene.
The findings, based on a new formula developed by the federal Centers for
Disease Control and Prevention, estimated that 4,762 New Yorkers contracted
H.I.V. in 2006, the most precise estimate the city had ever offered.
But the city stressed that because the method of estimating infections was new,
it could not be said definitively whether the number of new infections in the
city had increased or decreased from previous years.
Blacks, and men who have sex with other men, are the groups at greatest risk of
contracting H.I.V., the study found. A summary of the new data:
¶Men accounted for 76 percent of new H.I.V. infections and women for 25 percent.
(The figures exceed 100 percent because of rounding.)
¶Blacks made up 46 percent of the newly infected; Hispanics, 32 percent; and
whites, 21 percent. (Figures for other racial or ethnic groups were not
provided.)
¶Those under age 20 made up 4 percent of the newly infected; those 20 to 29
years old, 24 percent; those 30 to 39 years old, 29 percent; those 40 to 49
years old, 29 percent; and those 50 and older, 15 percent.
¶Sex between men was the main cause in 50 percent of new infections; high-risk
heterosexual sex in 22 percent; intravenous drug use in 8 percent; and unknown
or uncertain causes in 18 percent.
Manhattan accounted for 35 percent of new infections; Brooklyn, 26 percent; the
Bronx, 19 percent; and Queens, 17 percent.
As the health department has repeatedly noted, gay minority men were
particularly at risk. For example, of new H.I.V. infections among men under age
30 who have sex with men, 77 percent were in black or Hispanic men, as were 59
percent of new H.I.V. infections among men ages 30 to 50 who have sex with men.
Over all, the study found some interesting differences between national and
local rates of new H.I.V. infections.
Nearly two-thirds of the city’s new infections occurred in people 30 to 50 years
old. Nationally, people under 30 accounted for 41 percent of new infections,
compared with 28 percent in New York City.
Also, within New York City, whites were infected at four times the national
rate, Hispanics at three times the national rate, and blacks at almost twice the
national rate.
The health department said in a news release:
“The analytic technique is new, and the estimates may be imprecise, but even a
rough gauge of H.I.V. incidence is a valuable tool for understanding — and
combating — the spread of H.I.V. The health department’s new estimate includes
2006 incidence figures for different age groups, racial groups and both genders.
By repeating the exercise for subsequent years, researchers may be able to
discern increases and decreases over time, and target their prevention efforts
accordingly.”
Over the past year, the health department has warned that H.I.V. infections
among young gay men have risen and that unsafe sex remains common.
H.I.V. Is Spreading in New York City at Three Times the
National Rate,
a Study Finds, NYT, 27.8.2008,
http://www.nytimes.com/2008/08/28/health/research/28hiv.html
H.I.V.
Study
Finds Rate 40% Higher Than Estimated
August 3,
2008
The New York Times
By LAWRENCE K. ALTMAN
MEXICO CITY
— The United States has significantly underreported the number of new H.I.V.
infections occurring nationally each year, with a study released here on
Saturday showing that the annual infection rate is 40 percent higher than
previously estimated.
The study, conducted by the Centers for Disease Control and Prevention, found
that 56,300 people became newly infected with H.I.V in 2006, compared with the
40,000 figure the agency has cited as the recent annual incidence of the
disease.
The findings confirm that H.I.V., the virus that causes AIDS, has its greatest
effect among gay and bisexual men of all races (53 percent of all new
infections) and among African-American men and women.
The new figures are likely to strongly influence a number of decisions about
efforts to control the epidemic, said the disease centers’ director, Dr. Julie
L. Gerberding, and other AIDS experts. Timely data about trends in H.I.V.
transmission, they said, is essential for planning and evaluating prevention
efforts and the money spent on them.
Dr. Gerberding said the new findings were “unacceptable,” adding that new
efforts must be made to lower the infection rates. “We are not effectively
reaching men who have sex with men and African-Americans to lower their risk,”
she said.
Dr. Kevin A. Fenton, who directs H.I.V. prevention efforts at the agency, said,
“C.D.C.’s new incidence estimates reveal that the H.I.V. epidemic is and has
been worse than previously known.”
A separate historical trend analysis published as part of the study suggests
that the number of new infections was probably never as low as the earlier
estimate of 40,000 and that it has been roughly stable overall since the late
1990s.
C.D.C. officials said the revised figure did not necessarily represent an
increase in the number of new infections but reflected the ability of a new
testing method to more precisely measure H.I.V. incidence and secure a better
understanding of the epidemic.
Dr. Philip Alcabes, an epidemiologist at Hunter College in Manhattan, raised
questions about the validity of the findings. If they are true, Dr. Alcabes said
in a statement, the agency has undercounted new H.I.V. infections by about
15,000 per year for about 15 years. “Therefore, there are roughly 225,000 more
people living with H.I.V. in the U.S. than previously suspected,” he said. “The
previous estimate was 1 million to 1.1 million.”
A C.D.C. spokeswoman said Dr. Alcabes’s estimates were incorrect because the new
figures could not be used to calculate the total number of people with H.I.V.
The C.D.C. does not know the total number but is expected to determine it later
in the year.
The C.D.C., the federal agency responsible for tracking the AIDS epidemic in the
United States, said its new monitoring system provided more precise estimates
than were previously possible of new infections in specific populations.
Infection rates among blacks were found to be seven times as high as for whites
(83.7 per 100,000 people versus 11.5 per 100,000) and almost three times as high
as for Hispanics (29.3 per 100,000 people), a group that was also
disproportionately affected.
The C.D.C. has known of the new figures since last October, when the authors
completed a manuscript and sent it to the first of three journals. But the
agency refused to release the findings until they were published in a
peer-reviewed medical journal. The first two journals rejected the authors’
request for a fast-track review.
The paper is being published in the Aug. 6 issue of The Journal of the American
Medical Association. The journal and the disease centers had planned to release
it at a news conference on Sunday at the opening of the 17th International AIDS
Conference here. But the paper was released on Saturday because the embargo was
broken. A number of leading health experts have criticized the agency for not
releasing the information earlier. On Nov. 21, C.D.C. officials told AIDS
advocacy groups and reporters that the data would be released soon.
In an editorial on June 21, The Lancet, an internationally prestigious journal
published in London, severely criticized the disease centers for failing to
release the information and said, “U.S. efforts to prevent H.I.V. have failed
dismally.”
Dr. Gerberding, in defending the decision not to release the data earlier, said:
“This paper has been scrutinized by some of the best statisticians in the
country and is much better now than when we started this process. It was so
complicated that even I, who has some expertise in this area, could not stand by
it without making sure we had gone through the review process.”
She added, “This is one of those examples where getting the external review
process to really scrutinize the paper, pick it apart, build it back up, has in
my opinion fundamentally improved it.”
The delay, however, has also fueled criticism that the Bush administration,
which has earned plaudits for spending tens of billions to fight AIDS in a
number of highly affected countries, has not done enough to fight the disease at
home.
Representative Henry A. Waxman, Democrat of California and chairman of the
Committee on Oversight and Government Reform, was critical of the
administration. “H.I.V. prevention has been underfunded and too often hindered
by politics and ideology,” Mr. Waxman said in a statement released Saturday.
He said the administration had reduced domestic spending against H.I.V. “Since
fiscal year 2002, when adjusted for inflation, C.D.C.’s prevention budget has
actually shrunk by 19 percent. The president has recently requested decreases in
funding for H.I.V. prevention at C.D.C.”
Mr. Waxman said he would soon hold hearings on why health officials had had
“less and less money to actually get these programs to the communities that need
them.”
Dr. Alcabes disagreed with critics who contend that the new numbers point to a
failure of United States policy on AIDS, saying his conclusion was that “it
looks like prevention campaigns make even less difference than anyone thought.”
“H.I.V. incidence did not decline as much from the 1980s to the 1990s as we
believed,” he said, “despite the dramatic increase in condom promotion and
so-called prevention education.”
The C.D.C. said the findings confirmed sharp declines in the number of new
H.I.V. infections each year, from a peak of about 130,000 in the mid-1980s to a
low of roughly 50,000 in the early 1990s. But the findings also indicate that
the number of new infections increased in the late 1990s but has since remained
relatively stable, with estimates of 55,000 to 58,500 in the three most recent
time periods analyzed.
Dr. Gerberding said: “If there is any good news here, it is hard to report it,
but there is a little bit in the sense that while incidence rates are certainly
too high, they are stable. That is important because a stable number of new
infections in a world that has got more and more people with H.I.V. and people
with AIDS living in it suggests that we are keeping up with that pressure for
transmission.”
The revised figures are based on a new laboratory test that can distinguish
between recent and long-standing H.I.V. infection, as well as on statistical
measures and extrapolations.
The test is done in the laboratory on left-over serum from the standard H.I.V.
test after it shows that a person is infected. The Food and Drug Administration
has approved the test, known as BED.
Dr. Gerberding said that an earlier version of the new test was too crude to do
the same kind of study earlier this decade. Despite the improvements in the
test, she said, it is “not perfect yet.”
H.I.V. Study Finds Rate 40% Higher Than Estimated, NYT,
3.8.2008,
http://www.nytimes.com/2008/08/03/health/03aids.html
U.S. Blacks, if a Nation,
Would Rank High on AIDS
July 30, 2008
The New York Times
By LAWRENCE K. ALTMAN
If black America were a country, it would rank 16th in the world in the
number of people living with the AIDS virus, the Black AIDS Institute, an
advocacy group, reported Tuesday.
The report, financed in part by the Ford Foundation and the Elton John AIDS
Foundation, provides a startling new perspective on an epidemic that was first
recognized in 1981.
Nearly 600,000 African-Americans are living with H.I.V., the virus that causes
AIDS, and up to 30,000 are becoming infected each year. When adjusted for age,
their death rate is two and a half times that of infected whites, the report
said. Partly as a result, the hypothetical nation of black America would rank
below 104 other countries in life expectancy.
Those and other disparities are “staggering,” said Dr. Kevin A. Fenton, who
directs H.I.V. prevention efforts at the Centers for Disease Control and
Prevention, the federal agency responsible for tracking the epidemic in the
United States.
“It is a crisis that needs a new look at prevention,” Dr. Fenton said.
In a separate report on Tuesday, the United Nations painted a somewhat more
optimistic picture of the worldwide AIDS epidemic, noting that fewer people are
dying of the disease since its peak in the late 1990s and that more people are
receiving antiretroviral drugs.
Nevertheless, the report found that progress remained uneven and that the future
of the epidemic was uncertain. The report was issued in advance of the 17th
International AIDS Conference, which begins this weekend in Mexico City.
The gains are partly from the Bush administration’s program to deliver drugs and
preventive measures to people in countries highly affected by H.I.V.
The Black AIDS Institute took note of that program in criticizing the
administration’s efforts at home. The group said that more black Americans were
living with the AIDS virus than the infected populations in Botswana, Ethiopia,
Guyana, Haiti, Namibia, Rwanda or Vietnam — 7 of the 15 countries that receive
support from the administration’s anti-AIDS program.
The international effort is guided by a strategic plan, clear benchmarks like
the prevention of seven million H.I.V. infections by 2010 and annual progress
reports to Congress, the group said. By contrast, it went on, “America itself
has no strategic plan to combat its own epidemic.”
In a telephone interview, Dr. Fenton said, “We recognize this is a crisis, and
clearly more can be done.”
The institute, based in Los Angeles, describes itself as the only national
H.I.V./AIDS study group focused exclusively on black people. Phill Wilson, the
group’s chief executive and an author of the report, said his group supported
the government’s international anti-AIDS program. But Mr. Wilson’s report also
said that “American policy makers behave as if AIDS exists ‘elsewhere’ — as if
the AIDS problem has been effectively solved” in this country.
The group also chided the government for not reporting H.I.V. statistics to the
United Nations for inclusion in its biannual report.
Dr. Fenton said the C.D.C. had ensured that its data were forwarded to officials
in the Department of Health and Human Services and was investigating why the
data were not in the United Nations report.
Others speaking for the agency said the answer would have to come from the State
Department, which did not respond to an inquiry.
Dr. Helene Gayle, president of CARE and a former director of H.I.V. prevention
efforts at the disease control centers, told reporters on Tuesday that the
United States needed to devote more resources to care for people with sexually
transmitted diseases. Such infections can increase the risk of H.I.V. infection.
The federal government and communities needed to promote more testing among all
people, particularly blacks, to detect H.I.V. infection in its earliest stages
when treatment is more effective, Dr. Gayle said.
Also, she said, more needed to be done to promote needle exchange programs,
which have proved effective in preventing H.I.V. infection among injecting drug
users but that are illegal in many places.
The United Nations report said that in Rwanda and Zimbabwe, changes in sexual
behavior had led to declines in the number of new H.I.V. infections.
Condom use is increasing among young people with multiple partners in many
countries and more young people are postponing their initial sexual intercourse
before age 15.
The percentage of pregnant women receiving antiretroviral drugs to prevent
transmission of H.I.V. to their infants increased to 33 percent in 2007 from 14
percent in 2005. During the same period, the number of new infections among
children fell to 370,000 from 410,000.
The United Nations report affirmed treatment gains in Namibia, which increased
treatment to 88 percent of the estimated need in 2007, from 1 percent in 2003;
and in Cambodia, where the percentage rose to 67 in 2007 from 14 percent in
2004. Other countries with high treatment rates are Botswana, Brazil, Chile,
Costa Rica, Cuba and Laos.
In most areas of the world, more women than men are receiving antiretroviral
therapy, the report said.
Despite inadequate monitoring systems in many countries, data suggest that most
of the H.I.V. epidemics in the Caribbean appear to have stabilized. A few have
declined in urban areas in the Dominican Republic and Haiti which have had the
largest epidemics in the region.
Increased treatment was partly responsible for a decline in AIDS-related deaths
to an estimated 2 million in 2007 from 2.2 million in 2005.
The AIDS epidemic has had less overall economic effect than earlier feared, the
report said, but is having profound negative effects in industries and
agriculture in high-prevalence countries.
The United Nations has set 2015 as the year by which it hopes to reverse the
epidemic. But even if the world achieved that goal, the report said, “the
epidemic would remain an overriding global challenge for decades.”
To underscore the point, the United Nations said that for every two people who
received treatment, five people became newly infected.
U.S. Blacks, if a
Nation, Would Rank High on AIDS, NYT, 30.7.2008,
http://www.nytimes.com/2008/07/30/health/research/30aids.html
Editorial
The
Global AIDS Fight
February
29, 2008
The New York Times
Congress
and the White House are preparing to ramp up spending on programs to combat AIDS
and related diseases around the world while removing some of the ideological
blinders that have long undermined the effort to slow the spread of the AIDS
virus. It will be a welcome strengthening of a foreign aid program that was
already one of the shining accomplishments of the Bush administration.
The House Foreign Affairs Committee this week approved a bipartisan compromise,
crafted in negotiations between House leaders and the White House, that would
authorize a hefty $50 billion over the next five years to support campaigns
against AIDS, tuberculosis and malaria. This represents a huge increase over the
$19 billion appropriated in the first five years of the program and a
significant increase over the new funding requested by President Bush. The
president had originally proposed $30 billion over five years, primarily to
fight AIDS, whereas the new bill would authorize perhaps $37 billion to $41
billion to the AIDS struggle.
The administration’s program started small five years ago to meet a perceived
emergency as the AIDS epidemic spread out of control. It has already provided
drug treatment to almost 1.5 million men, women and children and supportive care
to millions of others. The focus for the next five years will be on making some
of the initial gains sustainable.
In one farsighted move, money will be used to train some 144,000 new health care
workers over the next five years to care for people infected with H.I.V., the
virus that causes AIDS. That is at best a start on easing the severe shortage of
health care workers in the developing world, which some estimates peg in the
millions. Other donor nations will need to contribute to the training effort as
well.
The most troublesome ideological constraint on the program — a requirement that
one-third of the funds used for prevention services be spent on abstinence
education — has been greatly eased. The bill calls for a balanced prevention
program that would promote abstinence until marriage and fidelity thereafter, as
well as condoms. It requires countries to report if abstinence and fidelity
funding falls below a certain percentage, but it sets no firm percentage that
has to be met.
The House is expected to pass the bill in the near future, and the Senate is
considering its own version. Although some Republicans are grumbling over the
amount of money proposed, it is important that Congress appropriate the full $50
billion if possible. Even that sum would almost certainly not provide universal
access to treatment for all people infected with H.I.V., a goal that the major
industrialized nations claim to be pursuing.
The Global AIDS Fight, NYT, 29.2.2008,
http://www.nytimes.com/2008/02/29/opinion/29fri1.html
This article is from a special (RED) edition
of The
Independent to mark World Aids Day
The suffering
that betrays a world divided
Published: 01 December 2006
The Independent
By Jonathan Brown, Andrew Grice
and Steve Bloomfield in Zambia
Today is World Aids Day. It was first marked in 1991, an
attempt by the international community to alert humanity to the terrible scale
of the threat posed by the disease.
Yet despite advances in medical science and a growing political consensus over
the need to act, the epidemic shows no signs of abating. In fact, it is getting
worse.
According to the United Nations, some 25 million people have already died from
Aids. A further 40 million men, women and children are living with HIV. Since
the turn of the millennium, 24.2 million people have been infected, 15.6 million
have died.
If the world continues on its present course, Aids is set to surpass the Black
Death of the 14th century as the deadliest outbreak of disease in human history.
World Aids Day will see millions marking their solidarity with those affected by
the virus. Charities, campaigners and politicians from Africa to the Americas
will speak of their plight and reveal the work that is going on to help them.
But the story of the battle against the epidemic reveals a world divided. A gulf
exists between sufferers living in poverty in sub-Saharan Africa and other parts
of the developing world and those in the rich nations of Europe and North
America.
The emergence of antiretroviral drugs, hailed by researchers as a "miracle" on a
par with the discovery of penicillin, means that in the affluent West at least,
HIV is now a treatable disease. The tragic irony is that in Britain infection
rates among some communities continue to rise. It was reported last week that
incidences among gay men had reached their highest level since 1981 as safe sex
practices were being ignored.
In Africa it is a different story. In Rwanda, where rapid advances in treatment
have helped hundreds of thousands, doctors call it the "Lazarus effect" - just
two antiretroviral drugs can restore a stricken patient to almost full health.
Costing less than a dollar a day, they can be bought from any corner shop.
The tragic irony here is that even at this price, they are too expensive. Africa
is seeing the fastest growth of any region of the world with an infection rate
of 15 per cent. Perhaps hardest hit are the 2 million HIV-affected children of
the region, who contracted the virus in the womb or during breastfeeding. Global
drug-makers have little interest in making smaller doses of their life-saving
medicines. The bigger profits are in the markets of the developed world among
the sick, rich adults.
So doctors in Africa are forced to crush adult pills into child-sized doses.
However, a deal will be announced today between two Indian drug-makers and
former US president Bill Clinton's foundation which promises to reduce
dramatically the cost of treating children infected with HIV-Aids next year.
But in some countries the threat of Aids is compounded by political failure. In
Zimbabwe, President Robert Mugabe has promoted traditional medicines over
antiretrovirals and displaced 1 million of his poorest urban citizens,
disrupting their treatment and increasing the infection rates in rural areas.
And even science has its limits. The hunt for a vaccine two decades after it was
claimed to be just five years away from completion remains as elusive as ever.
The British International Development Secretary, Hilary Benn, warned last night
that the world may miss its target of providing universal HIV prevention care
and treatment by 2010 unless the "stigma and prejudice" surrounding the disease
is tackled. "We mustn't let our discomfort or prejudice get in the way of saving
lives," he told a lecture at the London School of Economics to mark World Aids
Day.
However, the Government was condemned for its policy of deporting asylum-seekers
who are HIV positive back to their home countries, where treatment is often not
available. The Refugee Council said they should be given special dispensation to
stay.
Today is World Aids Day. It was first marked in 1991, an attempt by the
international community to alert humanity to the terrible scale of the threat
posed by the disease.
Yet despite advances in medical science and a growing political consensus over
the need to act, the epidemic shows no signs of abating. In fact, it is getting
worse.
According to the United Nations, some 25 million people have already died from
Aids. A further 40 million men, women and children are living with HIV. Since
the turn of the millennium, 24.2 million people have been infected, 15.6 million
have died.
If the world continues on its present course, Aids is set to surpass the Black
Death of the 14th century as the deadliest outbreak of disease in human history.
World Aids Day will see millions marking their solidarity with those affected by
the virus. Charities, campaigners and politicians from Africa to the Americas
will speak of their plight and reveal the work that is going on to help them.
But the story of the battle against the epidemic reveals a world divided. A gulf
exists between sufferers living in poverty in sub-Saharan Africa and other parts
of the developing world and those in the rich nations of Europe and North
America.
The emergence of antiretroviral drugs, hailed by researchers as a "miracle" on a
par with the discovery of penicillin, means that in the affluent West at least,
HIV is now a treatable disease. The tragic irony is that in Britain infection
rates among some communities continue to rise. It was reported last week that
incidences among gay men had reached their highest level since 1981 as safe sex
practices were being ignored.
In Africa it is a different story. In Rwanda, where rapid advances in treatment
have helped hundreds of thousands, doctors call it the "Lazarus effect" - just
two antiretroviral drugs can restore a stricken patient to almost full health.
Costing less than a dollar a day, they can be bought from any corner shop.
The tragic irony here is that even at this price, they are too expensive. Africa
is seeing the fastest growth of any region of the world with an infection rate
of 15 per cent. Perhaps hardest hit are the 2 million HIV-affected children of
the region, who contracted the virus in the womb or during breastfeeding. Global
drug-makers have little interest in making smaller doses of their life-saving
medicines. The bigger profits are in the markets of the developed world among
the sick, rich adults.
So doctors in Africa are forced to crush adult pills into child-sized doses.
However, a deal will be announced today between two Indian drug-makers and
former US president Bill Clinton's foundation which promises to reduce
dramatically the cost of treating children infected with HIV-Aids next year.
But in some countries the threat of Aids is compounded by political failure. In
Zimbabwe, President Robert Mugabe has promoted traditional medicines over
antiretrovirals and displaced 1 million of his poorest urban citizens,
disrupting their treatment and increasing the infection rates in rural areas.
And even science has its limits. The hunt for a vaccine two decades after it was
claimed to be just five years away from completion remains as elusive as ever.
The British International Development Secretary, Hilary Benn, warned last night
that the world may miss its target of providing universal HIV prevention care
and treatment by 2010 unless the "stigma and prejudice" surrounding the disease
is tackled. "We mustn't let our discomfort or prejudice get in the way of saving
lives," he told a lecture at the London School of Economics to mark World Aids
Day.
However, the Government was condemned for its policy of deporting asylum-seekers
who are HIV positive back to their home countries, where treatment is often not
available. The Refugee Council said they should be given special dispensation to
stay.
The suffering that
betrays a world divided, I, 1.12.2006,
http://news.independent.co.uk/world/science_technology/
article2029298.ece
This article is from a special (RED) edition
of The
Independent to mark World Aids Day
Defeating prejudice:
The red ribbon revolution
For quarter of a century,
campaigners have struggled to secure
funding
for the fight against Aids and HIV.
Stars rally to the cause now,
but it remains a tough battle.
Helen Brown reports
Published: 01 December 2006
The Independent
In the beginning
First there was fear. And confusion. Panic on the gay dancefloors of America. In
May 1981, The New York Times ran an article headlined: " Rare Cancer Seen in 41
Homosexuals". In 1982 the disease known as Gay Related Immune Deficiency was
renamed Acquired Immune Deficiency Syndrome, 1,300 new cases had been reported
in the US and 460 sufferers had died. That was the year that saw the first
support groups form: the Gay Men's Health Crisis in New York and the Aids
Project of Los Angeles. APLA's first big attempt at fundraising took place that
Christmas, with a benefit that netted $7,000. In 1984, a benefit concert at
Studio One featuring Joan Rivers raised $45,000.
And by the end of the decade, the organisation's tireless regime of campaigning
and benefit-organising had raised more than $77m for direct services for people
with Aids.
"Aids fundraising grew up at the same time as fundraising generally," Simon
Garfield, the author of The End of Innocence: Britain in the Time of Aids, says.
"In England, as in America, it began with small events in gay pubs and clubs. It
was all about 'how do we help our friends'. Everyone knew everybody else."
The close-knit community lent itself to telemarketing. "There was already a sort
of database," Mr Garfield says. "But people were nervous about how to get the
money. If you were collecting on the street, you had to make it clear that this
wasn't just about gay men. There were all these terrors of association which
took a few years to disperse."
However, celebrity support came slowly. "There was a lot of nervousness around
the issue for the big names," Mr Garfield recalls. "It was seen as just a gay
thing. Famous people who were openly gay were keen to support their friends. But
people like Elton John and George Michael were waiting to see which way the wind
blew. They were worried about the effect on their careers."
Inevitably, the deaths of celebrities had an impact. The matinee idol Rock
Hudson died of Aids in 1985, giving the disease "a face", in the words of Morgan
Fairchild. Then Freddie Mercury died in the UK in November 1991. "His death had
a huge effect and influence which spread far beyond the gay community," Mr
Garfield says.
The Terrence Higgins Trust
Terrence Higgins worked as a Hansard reporter in the House of Commons and as a
barman in the London nightclub Heaven. He collapsed while working at the club in
1982 and was admitted to St Thomas' Hospital, near Westminster, where he died of
pneumonia a few weeks later. He was 37 years old.
"We had no idea what was going on," Rupert Whitaker, Higgins's boyfriend at the
time, says. "We just knew that he was sick. I suggested to the consultant that
it was this new American disease. They ignored me. After Terry died they said to
me that I could read the autopsy report in the medical journals, but since I
wasn't family they wouldn't tell me directly. Terry had no family. I paid for
his funeral out of my student grant."
Martin Butler, a friend of Higgins, then approached Dr Whitaker. "He said, 'Why
don't we do something about this?'. I didn't want anyone else to go through what
I'd gone through. Martin's idea, originally, was to host club events. He was an
event organiser and he wanted to put together these club nights to fund research
and medical services.
"We put collecting tins in pubs. There were drag shows and donations. People
needed no prompting to give. People were starting to drop like flies. They would
be fine one day and three weeks later they would be dead. Everybody was
frightened. We didn't initially find many donors beyond the gay community
because of the huge stigma.
"We gave to the hospital where Terry had died," Dr Whitaker says. " But we
realised that supporting the existing services was a losing game; we needed to
provide support ourselves."
Tony Whitehead of the Terrence Higgins Trust (THT) says: "I had been
volunteering for the London Lesbian and Gay Switchboard and we were getting so
many calls from people who were frightened by news of Terrence's death. At the
end of a Switchboard meeting, I asked who wanted to form a group to do
something. We got together with Rupert and a group of Terrence's friends. And
the trust began in my flat in Marylebone. We wanted to become a proper charity
with all the legal and medical backing, with a focus on support and education."
The trust gained charitable status in 1984, the same year Mr Whitehead was
diagnosed HIV positive. "Although fundraising began in the gay community, we
forged links with other affected groups - we worked with people at the
Haemophilia Society because that got public attention," he says. "And we worked
with people who used drugs. Sometimes raising money was hard. Most people were
generous but a few had this ridiculous idea that HIV had been cooked up in some
germ laboratory to target the gay community. And others thought we were
exaggerating it and being anti-gay and anti-sex by speaking out. That seems
extraordinary now but I suppose when people are frightened they react in all
sorts of ways.
"We were fortunate in the appointment of Sir Donald Acheson as the Government's
chief medical Oficer," Mr Whitehead continues. "He knew this was going to be a
significant problem. So although getting government money was never easy, we did
get some. And as the media paid more attention the phone lines began ringing."
Debbie Holmes, the trust's head of fundraising, remembers her job interview.
"The panel said the job was hard. I thought they were overplaying it. I thought
that people were moved by the issue. But I am continually shocked by the
rejections we get and the hostility I face. People wrote vicious, homophobic
replies to our letters. The Charities Aid Foundation publish an annual ranking
for causes the public are most willing to support. And until last year, HIV/Aids
always came in at 25th out of 29. Now we're 15th out of 29."
Ms Holmes thinks that the public see what is happening overseas, but the problem
is not so visible at home. "People in the West don't 'look' so ill any more
because of the combination therapies. So it can be difficult to communicate the
human story. The struggle. The need."
"When Terrence became ill," Dr Whitaker says, "there was no co-ordinated medical
response. Treatment was, and still is, biomedical, not biopsychosocial. There
were no psychosocial services and ways of supporting people as they died, and
there's still very little of that. The quality of care here is dreadful, about
30 years behind the US. Which is why voluntary groups like the THT are still so
important."
Funding Fatigue
The National Aids Trust (NAT) was set up in 1987 by the Department of Health.
Its aim was to coordinate the HIV/Aids sector and one of its key aims was to
administer grants to other HIV/Aids organisations. Its chief executive, Deborah
Jack, says: "We used to be based in a government building, but we moved out in
1996. HIV was being de-prioritised. It was difficult to be sitting in the
Department of Health and challenging its policies."
Although World Aids Day, launched by the trust in 1991, provided an annual
public reminder, Dr Whitaker agrees about the de-prioritisation HIV/Aids issues
during the 1990s. "Physicians grabbed back control after the antiretrovirals
came in," he says. "We had volunteers in hospitals emptying bedpans because the
nurses wouldn't do it. But after the antiretrovirals came in, the volunteers
were kicked out and the issue became biomedical again. We're back full circle to
the idea that you've been 'bad' if you test HIV positive. There's this idea that
'the information's out there', but the information isn't out there. You get
16-year-olds saying, 'There are pills for that, I don't need to use a condom'."
NAT's government funding has been falling. "In 2003 we got £700,000 from the
government," Ms Jack says, "but in the year 2005/6 we got just £261,000. We're
having to look at other sources. Our biggest single source of income is
charitable trusts, a number of which have very specific objectives concerning
some of the most vulnerable groups in society.
"One of our frustrations is that most big companies have a 'charity of the
year', which closes the door immediately," she says. "HIV is never going to be
the 'big charity' of choice. Cancer charities, children's charities are always
more popular. And we've struggled to find companies to sell the red ribbons on
our behalf."
MAC Cosmetics, Levi's and Virgin are among the few companies selling ribbons in
store. And L'Oreal (which does work in the developing world using hairdressers
to educate clients about Aids) have been encouraging all hairdressers using
their products to sell ribbons.
"We couldn't get a corporate sponsor for World Aids Day this year," Ms Jack
says. "It would have been a good opportunity too. Last year, in the week around
World Aids Day, we had 5 million visitors to our website. There is undoubtedly,
depressingly, still stigma. I often say to people that the shape of the epidemic
has changed so much, the only thing that hasn't changed is the stigma. We still
read media reports about, say, a policeman being spat at by somebody HIV
positive, suffering 'an agonising wait for test results' although we should all
know you couldn't catch the virus that way.
"A poll found that one in three people living with HIV in the UK felt they had
suffered discrimination - and one of the biggest areas of discrimination was
health care, with dentists refusing to see people with HIV and GPs removing them
from their lists."
Spend and Save (Lives)
As the millennium passed, collecting tins began to ring hollow. A new impetus
was needed. Cue Bono, Bobby Shriver and Project RED: a plan to get the
corporations involved and the customer empowered. "Back in 1998," Mr Shriver
says, "there wasn't just funding fatigue in the US, there was nothing. Nobody
was paying attention. We didn't have Comic Relief. Bono and I started working in
America to develop some political muscle but in 2004 we realised we didn't have
any private sector support and that's where we came up with the idea for Product
RED. The colour's not based so much on the red ribbon as on the reality of Aids
as an emergency. We wanted to raise a red light - people are dying! Act now!"
RED is a brand, rather than a charity. With Mr Shriver as its chief executive,
it is licensed to partner companies such as American Express, Apple Computer,
Converse, Motorola, Gap and Giorgio Armani. Each company then creates a product
with the Product RED logo and a percentage of the profits from the sale of these
will go to the Global Fund to Fight Aids, Tuberculosis and Malaria. Amex has
promised to donate 1 per cent of every pound spent on its RED credit cards to
the fund. "The companies taking part are pretty brave," Mr Shriver says,
"because many, many more said no."
And he believes this "consumer power" will re-energise public engagement.
"People would come up to me or Bono and say that what we were doing was great,
how could they help? And we would say, 'Write a letter to the President, to your
senator, to Gordon Brown and Tony Blair'. But they don't want to do that. It
seems old fashioned or ineffective. But if you say to them, 'Would you get a
credit card if it were free and they gave half the money away?', people will do
that. If you're gonna get a credit card or a mobile phone or a T-Shirt anyway,
why not get a RED one?"
The idea is that, by making giving part of everyday life, those statistics will
not seem so insurmountable. Mr Shriver quotes Oscar Wilde: "It is the mark of a
truly educated man [or woman] to be deeply moved by statistics.
"But the numbers are there," he says, "and people aren't being moved by them or
they'd be behaving differently now. We've been in business six months in England
with the Motorola phone and the credit card and Gap have just launched their
collection. In America we've only been going five weeks. We're getting ready to
launch in Japan and the phones will launch in Nigeria, Malaysia, Singapore and
South Africa today. It takes time. Critics say, 'You should be launching in all
the world's countries simultaneously and set up the global fund right now', but
that's unrealistic. People have to give us a break and let us get it running."
Star Appeals
In April 1987, Diana, Princess of Wales became one of the first celebrities to
be photographed touching a person infected with HIV. "When so many still
believed that Aids could be contracted through casual contact," Bill Clinton
said in 2001, "Diana sat on the sickbed of a man with Aids and held his hand.
She showed the world that people with Aids deserve no isolation, but compassion
and kindness. It helped change world opinion, and gave hope to people with Aids
with an outcome of saved lives of people at risk."
Ms Jack of the NAT says Diana, who was the trust's patron from 1991 until her
death in 1997, was "incredibly powerful". "She made the issues come alive. She
dispelled the myths of transmission. The media don't see HIV/Aids as news. But
when a celebrity gets involved, they want pictures and we get headlines."
Other celebrities, such as Emma Thompson (who spoke of the "psychotic
detachment" of Western governments over the African Aids problem) and Stephen
Fry (who has been long involved with the THT) do much to keep the subject in the
news. When Scarlett Johansson spoke earlier this year about her own regular HIV
tests, she reawoke the topic in women's magazines.
And then there's Elton John, who established the Elton John Aids Foundation in
1992. The foundation has raised more than $100m to support programmes in 55
countries around the world.
Claire Lewis is Oxfam's international artist liaison manager. Her job is to
match the people who would prefer not to be called "celebrities" to Oxfam's
causes. "Lots of the artists we work with don't do much media. They do more
fundraising and advocacy. They'll host dinners and write letters. For example,
Helen Mirren will host a reception for a lot of lawyers or bankers and she'll
talk about her latest trip to Uganda. We won't ask for money then. But Helen
will send a letter later. A personal connection makes a difference."
Annie Lennox is just beginning work as one of Oxfam's ambassadors. " She's done
a lot of work with the HIV Aids Alliance and became very publicly associated
with the issue when she did a trip to Uganda for Comic Relief. We're trying to
raise £3m for HIV/Aids in Malawi and she provides a tangible figure. At the
moment she's doing voiceovers, adverts and writing letters."
The novelist Monica Ali has also used her name recognition to push HIV/Aids up
the public agenda. "I've been out to Uganda with Oxfam and to Calcutta with
Unicef," she says. "And I feel quite privileged to be in a position to do some
good.
"Sometimes you expect to be writing a horror story, about something overwhelming
which might make people feel powerless. But when I went out to Kampala the news
was relatively good. Lots of the people I met would have died 10 years ago,
before antiretrovirals were available. Just having the drugs isn't enough,
though. People can't always get to them, or there are problems for those who
have lost jobs and are trying to raise a family.
"As a novelist I've always been interested in the human angle and hopefully I
can report on the telling detail. Like the fact that antiretrovirals make you
very, very hungry. I didn't know that. But I was talking to the patients in
Kampala and they were laughing and saying that they'd be washing their hands
after a meal and they'd be ready to eat again."
As an ambassador for Unicef, Ewan McGregor has made a World Aids Day documentary
(to be shown on Sky Three at 8pm tonight) in which he visited Malawi to report
on children as the "missing face of Aids". He says: "I met children in Malawi
who have lost one or both parents to Aids and have been left to grow up alone.
In the run-up to Christmas and the New Year, don't buy your friends and family
the same old soap or socks. Why not buy one of Unicef's gifts instead? Last year
I bought my parents a ton of porridge for a village. For about £14, your could
give a child orphaned by Aids the basic health care, nutrition, school uniform
and supplies it needs, as well as psychosocial support during times of
distress."
Ribbons are Red, Ribbons are Blue and Kids Collect Shoes
In 1991, Jeremy Irons attended the Tony Awards with a little red loop pinned to
his lapel. He was the first high-profile celebrity to wear the red ribbon
created by the New York-based Visual Aids Artists Caucus earlier that year.
The trigger was a column by Michael Goff in the American gay/lesbian magazine
Outweek. Mr Goff had looked around at all the yellow ribbons worn in support of
the 1990-91 Gulf War, and he asked why there wasn't a ribbon for HIV/Aids. The
red was chosen as a "connection to blood and the idea of passion - not only
anger, but love, like a Valentine."
A visual symbol of an illness that many would rather not have mentioned, the red
ribbon was popular during the 1990s, and since there's no copyright on the red
ribbon, any HIV/Aids campaign can use it. But they're becoming less and less
visible. "We look quite enviously on breast cancer's pink ribbon now," Ms Jack
says. "Companies like M&S do so much for them. They do pink products. But we
can't get a dialogue going with red ribbons in the same way. We need a brave
company to stand up with us."
Last year Unicef launched the red and blue ribbon as part of its "Unite for
children, Unite against Aids" appeal. The aim is to to raise £15m for children
affected by Aids around the world by 2010. The charity has raised £2m since last
October.
Meanwhile, in association with Unicef, Blue Peter is helping children to get
involved in fundraising by donating old shoes to the Shoebiz Appeal for Malawi.
Defeating prejudice:
The red ribbon revolution, I, 1.12.2006,
http://news.independent.co.uk/world/science_technology/
article2029286.ece
This article is from a special (RED) edition
of The
Independent to mark World Aids Day
Why scientists
are still years from a vaccine
Published: 01 December 2006
The Independent
By Steve Connor, Science Editor
The unique nature of HIV has hampered the search for an Aids
vaccine and it remains a distant prospect, the world's leading experts say.
When American politicians announced the discovery of HIV in 1984, they predicted
that a vaccine and a cure for Aids would be available within five years. It
turned out to be a hopelessly optimistic assessment as the immense technical and
scientific difficulties unfolded.
Nevertheless, the discovery of the virus led to important developments. The
first was a blood test to determine whether someone was HIV positive. A global
research effort into the genetics and biology of HIV led to a deeper
understanding of the virus's modus operandi. This pointed to ways of sabotaging
viral replication in infected patients.
In the mid-1990s, the first clinical trials with a combination of antiviral
drugs demonstrated their immense potential as an effective form of treatment for
HIV-positive people.
Professor Jonathan Weber of Imperial College said the dramatic impact of
antiviral therapy transformed lives, but it did not solve the fundamental
problem of the growing epidemic. "Antivirals have increased the number of people
who are infected with HIV [by extending their lives] - but that's one of the
reasons why we still need a vaccine," he said.
There are, however, inherent problems with developing a vaccine against HIV. The
first is that it mutates rapidly, meaning that a vaccine developed against one
form of the virus may not work against another. Another problem is that HIV
integrates itself into the DNA of an infected person. A third difficulty is that
the virus attacks the very cells of the immune system sent to attack it. Once
infected, these T-cells take the virus deeper into the body's immune defences.
Albert Sabin, who developed the world's first oral polio vaccine, said in 1993
that he thought the problems posed by HIV would make it impossible to produce an
effective Aids vaccine. He was proved right. The only putative Aids vaccine to
reach the final of clinical trials was shown to be a dud in 2004.
In recent years, however, the focus of vaccine development has shifted. Instead
of trying to produce a vaccine to prevent infection, scientists are hoping to
develop a vaccine to prevent the onset of Aids in people who are HIV positive.
These therapeutic vaccines are aimed at stimulating the disease-fighting cells
of the immune system rather than its prophylactic antibodies. Merck, the US
pharmaceuticals company, is leading the effort with a vaccine based on a
genetically modified virus with three HIV genes. The US National Institutes of
Health and a European consortium both have their own initiatives, with the help
of government sources and private organisations such as the Bill and Melinda
Gates Foundation.
However, few experts are predicting an Aids vaccine is around the corner. Andrew
McMichael, professor of molecular medicine at Oxford University, who is leading
Britain's vaccine effort, said: "I'm optimistic we'll get to it eventually, but
I'm not optimistic about having a solution in three or four years."
Why scientists are
still years from a vaccine, I, 1.12.2006,
http://news.independent.co.uk/world/science_technology/
article2029296.ece
This article is from a special (RED) edition
of The
Independent to mark World Aids Day
The Big Question:
What do we really know about Aids?
Published: 01 December 2006
The Independent
By Ben Chu
Remind me, what exactly is Aids?
Aids stands for Acquired Immune Deficiency Syndrome. This is a broad description
of a variety of symptoms displayed by someone who has been infected by the Human
Immunodeficiency Virus (HIV). It usually takes about a decade for someone who is
"HIV positive" to develop full-blown Aids. Once they are infected, they are
infected for life.
What does it do to the body?
The virus itself does not kill. HIV attacks a person's immune system, our
natural defence system, fatally weakening it over time. To be more precise, HIV
sabotages a specific immune cell, known as CD4 lymphocyte. This makes Aids
sufferers especially vulnerable to infections. People with Aids often succumb to
illnesses such as pneumonia that a healthy person would normally be expected to
fight off. Without treatment, the average survival time after developing Aids is
10 months, but in individual cases it can range from two weeks up to 20 years.
Where did it come from?
Wild chimpanzees is the most likely theory. Cases of human infection were
recorded in Kinshasa, the capital of the Democratic Republic of Congo, in the
1930s. It is believed that people hunting chimpanzees in neighbouring Cameroon
may have contracted a mutation of the Simian Immunodeficiency Virus (SIVcpz)
that managed to jump the species barrier.
Earlier this year, a team of scientists from the universities of Nottingham,
Montpellier and Alabama identified a natural reservoir of SIVcpz in chimpanzees
in southern Cameroon. According to Paul Sharp, professor of genetics at the
University of Nottingham: "When you consider that HIV probably originated more
than 75 years ago, it is most unlikely that there are any viruses out there that
will prove to be more closely related to this human virus."
Why did it take so long for us become aware of it?
The relative rarity of cases and the fact that symptoms differ significantly
between individuals meant the virus was not identified for another half a
century. The condition first came to public attention when gay men in the United
States began dying of routine illnesses in unusually large numbers. On 5 June
1981, the US Centers for Disease Control and Prevention recorded a cluster of
pneumonia in five homosexual men in Los Angeles. So strong was the apparent link
with homosexuals that it was at first labelled "Gay Related Immune Deficiency".
But when it became clear that half of those affected were not gay, the term Aids
was coined. The scientific breakthrough came in 1983 when HIV was isolated by
Luc Montagnier of the Pasteur Institute in Paris, and then a year later it was
confirmed by Robert Gallo of the US National Cancer Institute.
How prevalent is it?
Aids is a pandemic. According to the World Health Organisation and Unaids, the
Joint United Nations Programme on HIV/Aids, some 40 million people are living
with HIV around the world. And more than 25 million people are estimated to have
died since 1981 as a result of Aids-related diseases. In 2005, around 2.8
million people died of Aids-related illnesses, 570,000 of them children.
Meanwhile, approximately 4.1 million people were newly infected.
Sub-Saharan Africa is easily the worst affected region, with between 21 million
and 28 million people suffering, 64 per cent of the world's total. But numbers
in eastern Europe and Asia continue to rise. Ukraine and Russia are particularly
badly hit. And India has overtaken South Africa as the country with the highest
number of sufferers within its borders. In the UK, US and western Europe levels
of infection have stabilised, but are showing disturbing signs of a resurgence
in the gay community.
How is it transmitted?
The virus is passed through blood, semen, vaginal fluids and breast milk.
Unprotected sexual intercourse with an infected person is the most common method
of transmission. It can also be spread by contact with infected blood. HIV can
cross from mother to child during pregnancy, childbirth or breastfeeding.
Another common route is the sharing of needles. A person cannot catch HIV from
toilet seats, or by touching, hugging or shaking hands with an affected person.
Is there a cure?
No. Scientists are working to find a vaccine, though 25 years of research has
yet to yield any significant breakthrough. But HIV need not be an imminent death
sentence anymore. There have been major advances in HIV treatment development.
In 1996, highly active antiretroviral therapy (Haart), a daily cocktail of
drugs, was introduced. This stabilises a patient's symptoms. The result is that
many people, although by no means all, can now live with HIV for decades.
Despite unpleasant side-effects such as nausea and diarrhoea, many of those
taking these drugs have experienced a vast improvement in their general health
and quality of life.
How can it be prevented?
Using a clean needle for the injection of drugs and using condoms in sexual
intercourse. Resistance, or ignorance, with regard to the second has been the
most significant contributor to the rapid spread of HIV around the world. The
Catholic Church has come in for a good deal of criticism for its opposition to
the use of condoms on religious grounds.
How have public attitudes to the illness changed over the
years?
Fundraising and lobbying by the gay community forced the media to take notice.
In 1987, the National Aids Trust was set up by the Department of Health, and the
Government launched its famous "Don't die of ignorance" campaign. The
photographing of Princess Diana embracing an HIV sufferer in the same year did
an enormous amount to lift the stigma from the condition.
The deaths of high-profile Aids victims such as Rock Hudson in 1985 and Freddie
Mercury in 1991 also heightened awareness. The first international World Aids
Day was held in 1988. The annual event has successfully projected Aids as a
global problem, requiring a global solution.
Are there any grounds for hope?
Some. A survey by Unaids of 126 countries this year found the rate at which
people are infected with HIV may have peaked in the late 1990s. The incidence of
new HIV infections in some countries seems to have stabilised for the first time
in 25 years. Six out of 11 African countries reported declines of at least 25
per cent in HIV prevalence among 15- to 24-year-olds in capital cities.
And this year Bill Gates, below, the world's richest man, pledged $287m (£155m)
to try to speed up the development of a vaccine for the HIV/Aids virus. The
money is being split into 16 grants for science teams across the world - with
the aim that they work more collaboratively on new approaches. All the
recipients have had to agree to share their findings - even if they had been
working on competing projects. There are also signs that the Catholic Church is
preparing to liberalise its views on condoms, which could have a significant
impact on reducing the rates of infection among Africa's Catholic communities.
So have we reached a turning point?
Far from it. Many millions continue to die needlessly because antiretroviral
drugs are extremely expensive and not widely available in many poor countries,
despite the fact that it is in poor countries where Aids is most widespread. And
drug companies are still resistant to the widespread production of cheaper
generic versions of their patented antiretroviral drugs.
A UN target of getting antiretroviral therapy to three million people by 2005
was missed. Only one in five people around the world gets the drugs they need.
Vast numbers will continue to be infected through ignorance too. The UN's
Declaration of Commitment on HIV/Aids wanted 90 per cent of young people around
the world to know about the disease by 2005. But surveys show that fewer than
half have comprehensive knowledge of the nature of Aids and how to avoid it.
The Big Question:
What do we really know about Aids?, I, 1.12.2006,
http://news.independent.co.uk/world/science_technology/
article2029236.ece
This article is from a special (RED) edition
of The
Independent to mark World Aids Day
RED campaign offers
thousands of Aids sufferers
the
'Lazarus effect'
Published: 01 December 2006
The Independent
By Julia Stewart
When Bono visited the paediatric ward of the central hospital
in Kigali last May, eight-year-old Denyse Mushimiyimana was almost comatose.
Newly diagnosed with HIV, her tiny skeletal frame lay motionless on her bed
while her distraught father, who is also infected, sat at her bedside. She
didn't utter a word. Three months later, Denyse was back at her Rwandan school
in a neatly pressed uniform, laughing and skipping as usual with her friends.
Her parents are naturally delighted.
Denyse is an example of the Lazarus effect of antiretroviral therapy. "Aids is
no longer a death sentence," Bono said. "Just two pills a day will bring someone
who is at death's door back to full health, back to full life. Doctors call it
'the Lazarus effect'. I've seen it myself and I have to say that it's nothing
short of a miracle. These pills are available at any corner drugstore. They cost
less than a dollar a day, but the poorest people in Africa earn less than a
dollar a day. They can't afford them, and so they die. It's unnecessary. It's
insane."
In view of this, last March, Bono and the philanthropist Bobby Shriver launched
a campaign called RED to allow big businesses and customers to contribute to the
fight against HIV and Aids. So far, six companies have joined up - Amex, Apple,
Armani, Gap, Converse and Motorola - and brought out RED products.
A percentage of sales is donated to the Global Fund, an independent organisation
set up in 2002 to fight Aids, TB and malaria. Motorola, for example, donates £10
for every RED phone bought, as well as 5 per cent of the purchaser's monthly
bill. Gap and Armani donate 50 per cent of the profit from their RED
collections.
Donations from RED products are specifically used to combat Aids in Africa. Just
over $10m (£5.1m) has been raised so far. "The RED campaign is one of the most
exciting and hopeful things that has happened in the five years that the Global
Fund has existed," said Professor Richard Feachem, executive director of the
Global Fund. "Through it major corporations and ordinary men and women all over
the world are engaging positively and constructively in the fight again HIV/Aids
in Africa."
About $6m has gone to Rwanda and $4m to Swaziland to support programmes
particularly aimed at women and children. In Rwanda it is being used to increase
testing and the availability of treatment. Antiretroviral therapy now costs
about $140 per person per year, compared with $10,000 in 2000. The dramatic
reduction in cost is a result of the Global Fund buying huge amounts of drugs
for people too poor to buy them, as well as the Clinton Foundation's price
negotiations with the Indian drug manufacturers.
Not only are drugs cheaper, they are much easier to take. Five years ago,
patients had to take numerous different pills at varying stages of the day.
Treatment now is two pills a day. Rwanda's compliance rate - the ability of
patients to take medicine properly - is now higher than in the UK or US.
"The RED money is helping roll out this revolution in Rwanda, scaling up this
affordable and feasible treatment," Professor Feachem said. "What that does is
give decades of life to people who would otherwise die quickly. The so-called
Lazarus effect is when you see a man, woman or a child, who is within weeks or
days of death, and who looks like a walking skeleton, and you put them on
antiretroviral therapy and they regain their health in a most amazing way. Four
or six weeks later there is already a big difference. After three months you see
a very big difference: the child is back in school and the parent is a parent
again and back at work."
Much of the money donated to Swaziland will be spent on orphans. The country has
the world's highest HIV/Aids rate. Among those aged 15 to 50, it is 33 per cent,
and for women aged 25 to 30, the figure is over 50 per cent. One of the impacts
of this "viral genocide" is a huge numbers of orphans, about 70,000 in a
population of one million.
Already 37,000 orphans are receiving food and assistance to attend school,
supported by the Global Fund. Instead of children having to go to orphanages,
277 KaGogo (meaning granny) centres have been set up. Grandmothers are given
financial support to feed orphans and provide schooling. As children stay in
their community they are at less risk of being abused.
The RED money is also being used to expand testing and treatment. Dr Derek von
Wissell, director of NERCHA, Swaziland's statutory HIV and Aids programme, said
the money had had a huge effect. In 2001 the government spent about one million
rand (£75,000) on HIV and Aids. This year it is hoping to spend about 150
million, 110 million of it from the Global Fund. "Free treatment only started
being available in 2003. Before that people had to pay for it privately. We now
have between 15,000 and 16,000 patients," he said. "I personally know a large
number of people who were virtually dying who are back at work, completely
functional and looking after their families."
Tembi Nkambule, 32, is one whose life has been drastically improved by
medication.
The mother-of-three, who lives in Manzini, about 20 miles from the capital
Mbabane, said: "It has made so much difference for me. I'm always fine and
sometimes I even forget that I have HIV. I feel so well I'm sure I still have
more years to live."
RED campaign offers
thousands of Aids sufferers the 'Lazarus effect' ,
I, 1.12.2006,
http://news.independent.co.uk/world/
science_technology/article2029294.ece
This article is from a special (RED) edition
of The
Independent to mark World Aids Day
Fergal Keane:
The spirit of resistance that has found
a new
voice in the struggle against Aids
You could watch coffin follow coffin into the earth.
Death was
knocking on doors everywhere
Published: 01 December 2006
The Independent
I can't exactly recall when I became aware of HIV/Aids in
South Africa. I think it was at the start of the 1990s, when we began to get
calls from women's groups in the townships. "Come to our demonstration. We are
handing out leaflets and condoms," they would say. I went to one demonstration
in Alexandra township down the road from where I used to live in Johannesburg. I
remember enthusiastic women in a small procession and a bemused local populace.
And that was really the extent of it. I did go to Zimbabwe in those years and
visited an AIDS hospice run by Irish nuns. There were about seven or eight
people there being cared for with great gentleness. And I remember one of the
nuns saying one of the worst problems was the stigma. People just didn't want to
face up to the problem.
But like most of the other journalists covering the region back then, I was
preoccupied with the epic story in South Africa. Mandela had been released from
prison. There was terrible violence in the townships. It was an exciting and
often frightening time. In those days I used the phrase " the heave of history"
to describe the tumultuous transition. What I and so many others missed,
however, was the insistent march of HIV. Go back now and read, listen or watch
the coverage of South Africa in those years and you will really struggle to find
any sense of HIV/Aids as a devastating crisis.
That was largely because the political imperative was finding a solution to a
conflict which could have pitched South Africa into a civil war. There were
other factors: the white regime never seemed overly concerned about a disease
which largely affected the black population; the older ANC leaders such as
Mandela betrayed a deep reluctance to confront sexual matters. But these were
secondary to the main problem of preventing a racial bloodbath.
And then came 1994. The transcendent moment when a democratic South Africa was
born, and along with it came a whole new list of reasons for not making Aids a
priority. I deliberately use the word "reasons" and not " excuses". There were
houses and schools to build, water and electricity and jobs to provide. Yes Aids
was a growing problem, and one that the politicians were by now well aware of.
Journalists were highlighting the issue as were the increasingly concerned
health professionals.
Others can disagree but I think it's reasonable to cut the politicians some
slack in those early years. They can make a plausible defence for failing to
push Aids to the top of their priority list. Where the excuses run out is after
two or three years of the new government, when political and economic stability
had been achieved and there was time to reflect on the bigger picture.
By the late 1990s, that picture was very bleak indeed. You could go into
hospitals all over the country and see the gaunt figures of Aids victims and
hear their rasping, tubercular coughs. You could travel to Soweto's main
cemetery at the weekend and watch coffin follow coffin into the newly turned
earth. Death was knocking on doors in every part of the country.
Enter a new president. I remember writing in this paper in fairly hopeful terms
about Thabo Mbeki when he was first elected back at the end the 1990s. He was a
technocrat, a politician who had proved wise in the long negotiations to end
white rule, and who had come to power promising to improve the daily lives of
the poor. In beginning the work of creating equality, Mbeki has done well. To
anybody who knew the old South Africa, that land of oppression and humiliation,
the modern country is by far a happier and better place.
But with one huge exception. For Mbeki's record on Aids is bleak: a refusal to
recognise the scale of the problem, flirting with the science of the HIV/Aids
deniers and verbal attacks on those who were bold enough to contradict him.
Three years ago, he caused outrage by saying in New York that he personally did
not know anybody who had been diagnosed with HIV. This from the leader of a
country where one in 10 of the population was estimated to be HIV positive, and
whose own spokesman had died after a lengthy illness after being diagnosed with
HIV.
Yet the official confusion has continued. Just when it seemed the government was
taking a more enlightened approach the health minister, Dr Manto
Tshabalala-Msimang, told an international conference last August that garlic,
beetroot and African potatoes were effective in managing the disease. According
to one report, the South African government stand in the conference hall
featured a display of vegetables but no antiretroviral drugs.
Of course they are not a cure for Aids. Nor will they rid South Africa of the
poverty, the lack of power among rural women and the attitudes towards sex which
have allowed HIV/Aids to thrive. But they do make a real difference to the lives
of those for whom they are properly proscribed and who are carefully monitored.
During that last trip to South Africa, I went to a small house in the Eastern
Cape that serves as an Aids clinic. Inside I was confronted immediately with
those iconic images of Aids in Africa: the figures prostrate beneath thick
woollen blankets, the look in the eyes that is halfway between despair and
resignation. I was taken back to that other house in Zimbabwe a decade earlier.
And yet it was here among the dying and the severely ill that a little glimmer
of hope appeared. It came, as so often in my experience of Africa, from a woman.
Lulu Boxosa runs the Aids charity Temba and campaigns not only for funds but to
open eyes and ears to the catastrophe that has attacked so many homes. Lulu is
not bitter about the official failures. She doesn't have time for that.
Everybody woke up too late, she told me. But her presence, the bustling good
humour she brings into the rooms of the dying, speaks of one of South Africa's
greater advantages, the power of civil society. Apartheid bequeathed a terrible
legacy of poverty, but it also created a tradition of resistance which has found
a new voice in the fight against Aids.
Those like Lulu - and there are so many like her across Africa - know that
speaking out unambiguously about what causes Aids and what can manage the crisis
is where any successful campaign must begin. She is not so naïve as to think
that a well-managed roll-out of drugs or a campaign to change sexual behaviour
will bring this tragedy to an end. But she knows these are the vital first
steps.
If the fight against apartheid taught us anything it is that South Africa's
grassroots campaigners don't give up. There are already signs that senior ANC
figures will respond to the pressure. On World Aids day, amid the plentiful
images of sorrow, that spirit is a small, good thing to remember.
Fergal Keane is a BBC Special Correspondent.
His series 'Taking A Stand' is
broadcast on Radio 4
on Tuesdays at 9am
Fergal Keane: The
spirit of resistance
that has found a new voice in the struggle against Aids, I,
1.12.2006,
http://comment.independent.co.uk/commentators/article2029240.ece
- broken link
This article is from a special (RED) edition
of The
Independent to mark World Aids Day
How the world's drug firms
sacrificed profits in the battle
against Aids
The Independent
Published: 01 December 2006
By Karen Attwood
Being handed an HIV-positive diagnosis is no longer a death
sentence in the West. HIV/Aids, though a chronic illness, is manageable. With
varying combinations of antiretroviral drugs (ARVs) and careful monitoring by
the medical profession, an HIV/Aids patient can expect to live for many years.
Yet in the developing world the picture is entirely different. Communities are
being wiped out and economies destroyed. In Sub-Saharan Africa, where 25.3
million people are estimated to have been affected, life expectancy, which had
risen from 44 to 59 between the 1950s and 19902, has dropped back to below 45.
Wind back six years and the big pharmaceutical companies were being blamed for
the chaos brought on by the onslaught of Aids in the developing world.
There was a siege of bad publicity. The public couldn't understand why highly
profitable drug companies were allowing millions to die because they insisted on
upholding their patents and wouldn't give away free drugs. By not allowing
poorer countries to make cheaper generics of AVRs, they were accused of having
blood on their hands.
Drug firms argued that giving away free drugs was detrimental. It takes a
massive $800m and 10 to 15 years of research and development to get a drug to
market. If firms do not make a profit from their products, research and
development (R&D) dries up and there are no more developments for the greater
benefit of mankind. It is vital for the survival of a company that intellectual
property is protected.
As Richard Ley, a spokesman for the Association of the British Pharmaceutical
Industry, says: "It would be easy for us to dump lots of medicine and say we
have done our bit but that is no going to solve any problems."
One pharmaceutical analyst pointed out that if you give drugs away for free you
are faced with the problem of "flowback". "If you have free access to HIV
treatments it can find its way into other markets pretty quickly," he said.
Jon Pender, the director of government affairs access issues and intellectual
property at GlaxoSmithKline, the UK's largest drug company, formed from the
merger of Glaxo Wellcome and Smithkline Beecham in 2000, said the tie-up between
the firms came at the time of the highly politicised debate on Aids, when the
drug firms were being demonised. It was an opportunity to change tack.
The new chief executive Jean Pierre Garnier decided GSK was not going to focus
on the world's richest nations. The industry's reputation had suffered but also
the business model needed to be protected. So what solutions did the major drugs
firms come up with?
In 2001, seven firms - GSK, Abbott, Merck & Co, Bristol-Myers Squibb, Roche,
Gilead Sciences and Boehringer Ingelheim, joined forces with the UN to look at
ways in which they could bring prices down in the developing world. Mr Pender
said one step forward was the decision to sell drugs to developing countries at
"not-for-profit" prices.
Further reaching still was the creation of a system of voluntary licensing,
where companies were given the know-how to create AVRs without the need for a
patent. GSK has so far granted seven voluntary licenses, including to Aspen
Pharmacare, Africa's largest manufacturer of generic drugs.
"The need was so great out there that enabling more companies to supply these
products, the better," Mr Pender said. "The firms see this as a commercial
activity. They want to do something to improve the situation in Africa but it is
a commercial opportunity."
However, having cheap AVRs does not solve HIV. What makes it different from
other chronic yet treatable diseases is that strains of the virus become
resistant and new drugs need constantly to be developed, fuelling the need for
more money for R&D.
ARVs work by blocking viral replication within existing cells at different
stages in the life cycle of the virus. Although US firm Merck & Co is the
closest to a vaccine and is about to begin stage-three trials, this is still 10
to 15 years away. The pressure remains and the research continues. Just this
week, a small Australian biotech, Virax, which has been working on vaccine
development for 20 years, announced it has agreed funding with eight
international mining companies, including BHP Billiton and Rio Tinto, for trials
which will take place in South Africa for it's a HIV/Aids therapeutic vaccine.
The proposed trial will involve 140 HIV-positive subjects in five established
HIV clinics. The chief executive of Virax, Dr David Beames, said: "The totally
new and innovative funding model for the product development has enormous
potential for application to a whole range of other diseases of the
emerging/developing world that would otherwise be ignored.
"Southern Africa is the epicentre of the HIV pandemic. The sooner trials/drug
development commences here the sooner it could, if successful would become
available as a treatment."
Dr Vinh-Kim Nguyen, from the Department of Social and Preventive Medicine at the
University of Montreal, who visited London this week to give a lecture at UCL,
in the run-up to World Aids Day, said: "It is not the drugs companies that are
the problem. They have to make money for their shareholders and provide drugs
where there are markets and they do that well. The problem is when it comes to
comes to global public health, there is no market for drugs for poor people."
Dr Nguyen argues that the whole structure and the way we deal with healthcare in
the developing world needs to be rethought. Debt relief would go some way to
solving the funding issue, he said.
"The real problem is governments," he said.
The most recent report from Unaids and the World Health Organisation revealed
that the total number of people still infected stand between 34 millionand 47
million. In Asia and Central Europe new infections has risen by 70 per cent in
two years. And although new infection rates are levelling out in some countries,
such as Lesotho, in Uganda where the epidemic had been brought under control,
rates are rising again. Some say this is due to a shift in American government
policy away from giving out free condoms to promoting abstinence.
Justine Frain, from GSK's Community Partnership programme, says that a key
aspect of the drug industry's response to the Aids crisis is providing funding
to voluntary organisations that work on the ground. Stigma and discrimination
are massive barriers to people getting tested. There are cases of HIV positive
mothers continuing to breastfeed their babies as they do not want the community
to know they are HIV positive, she said.
GSK works with NGOs across 20 countries and has spent £70m in 11 years on
community projects. "This is a key aspect of GSK's response to Aids," Ms Frain
said. "It is to support communities to help themselves."
Sine 2000, the global drugs industry has donated £2.5bn to the developing world
to help treat 539m people through various projects.
Mr Ley, from the ABPI, said the fight against AIDS in poorer countries is made
so much more difficult due to the lack of infrastructure, education and basic
facilities. Malnutrition, the lack of clean water and the prevalence of TB and
malaria compound the misery and ensure that once HIV takes hold, a victim can
succumb far more quickly that in the west.
"To ensure that patients receive treatment the infrastructure needs to be
there," Mr Ley says. "This is not something we can solve by ourselves as an
industry. It can only be done in partnership."
The Aids pipeline
* There are 77 HIV/Aids medicines and vaccines in clinical trials
or submitted
for approval in the US alone
* Eighty-eight HIV/Aids medicines registered already,
including 22 ARVs
* Nineteen vaccines are in the pipeline
* It costs $800m to develop one medicine
* Only one in ten vaccines in the pipeline will make it
into an actual vaccine
* The US drugs industry spent $39.4bn on R&D in 2005
How the world's drug
firms sacrificed profits in the battle against Aids,
I,
1.12.2006,
http://news.independent.co.uk/business/
analysis_and_features/article2029303.ece - broken link
AIDS Toll May Reach
100 Million in Africa
June 4, 2006
Filed at 1:32 a.m. ET
The New York Times
By THE ASSOCIATED PRESS
JOHANNESBURG, South Africa (AP) -- It began quietly, when a
statistical anomaly pointed to a mysterious syndrome that attacked the immune
systems of gay men in California. No one imagined 25 years ago that AIDS would
become the deadliest epidemic in history. Since June 5, 1981, HIV, the virus
that causes AIDS, has killed more than 25 million people, infected 40 million
others and left a legacy of unspeakable loss, hardship, fear and despair.
Its spread was hastened by ignorance, prejudice, denial and the freedoms of the
sexual revolution. Along the way from oddity to pandemic, AIDS changed they way
people live and love.
Slowed but unchecked, the epidemic's relentless march has established footholds
in the world's most populous countries. Advances in medicine and prevention that
have made the disease manageable in the developed world haven't reach the rest.
In the worst case, sub-Saharan Africa, it has been devastating. And the next 25
years of AIDS promise to be deadlier than the first.
AIDS could kill 31 million people in India and 18 million in China by 2025,
according to projections by U.N. population researchers. By then in Africa,
where AIDS likely began and where the virus has wrought the most devastation,
researchers said the toll could reach 100 million.
''It is the worst and deadliest epidemic that humankind has ever experienced,''
Mark Stirling, the director of East and Southern Africa for UNAIDS, said in an
interview.
More effective medicines, better access to treatment and improved prevention in
the last few years have started to lower the grim projections. But even if new
infections stopped immediately, additional African deaths alone would exceed 40
million, Stirling said.
''We will be grappling with AIDS for the next 10, 20, 30, 50 years,'' he said.
Efforts to find an effective vaccine have failed dismally, so far. The
International AIDS Vaccine Initiative says 30 are being tested in small-scale
trials. More money and more efforts are being poured into prevention campaigns
but the efforts are uneven. Success varies widely from region to region, country
to country.
Still, science offers some promise. In highly developed countries, cocktails of
powerful antiretroviral drugs have largely altered the AIDS prognosis from
certain death to a manageable chronic illness.
There is great hope that current AIDS drugs might prevent high-risk people from
becoming infected. One of these, tenofovir, is being tested in several
countries. Plans are to test it as well with a second drug, emtricitabine or
FTC.
But nothing can be stated with certainty until clinical trials are complete,
said Anthony Fauci, a leading AIDS researcher and infectious diseases chief at
the U.S. National Institutes of Health.
And then there is the risk that treatment will create a resistant strain or, as
some critics claim, cause people to lower their guard and have more unprotected
sex.
Medicine offers less hope in the developing world where most victims are
desperately poor with little or no access to the medical care needed to
administer and monitor AIDS drugs. Globally, just 1 in 5 HIV patients get the
drugs they need, according to a recent report by UNAIDS, the body leading the
worldwide battle against the disease.
Stirling said that despite the advances, the toll over the next 25 years will go
far beyond the 34 million thought to have died from the Black Death in 14th
century Europe or the 20 to 40 million who perished in the 1918 Spanish flu
epidemic.
Almost two-thirds of those infected with HIV live in sub-Saharan Africa where
poverty, ignorance and negligent political leadership extended the epidemic's
reach and hindered efforts to contain it. In South Africa, the president once
questioned the link between HIV and AIDS and the health minister urged use of
garlic and the African potato to fight AIDS, instead of effective treatments.
AIDS is the leading cause of death in Africa, which has accounted for nearly
half of all global AIDS deaths. The epidemic is still growing and its peak could
be a decade or more away.
In at least seven countries, the U.N. estimates that AIDS has reduced life
expectancy to 40 years or less. In Botswana, which has the world's highest
infection rate, a child born today can expect to live less than 30 years.
''Particularly in southern Africa, we may have to apply a new notion, and that
is of `underdeveloping' nations. These are nations which, because of the AIDS
epidemic, are going backwards,'' Peter Piot, the director of UNAIDS, said in a
speech in Washington in March.
Later, at a meeting in Abuja, Nigeria, last month, Piot cited encouraging news
including a sharp fall in new infections in some African countries. There also
has been an eightfold increase in the number of Africans benefiting from
antiretroviral treatment, he said.
But, he warned, ''the crisis of AIDS continues and is getting worse and any
slackening of our efforts would jeopardize the hard-won gains of each and every
one of us.''
Besides the personal suffering of the infected and their families, the epidemic
already has had devastating consequences for African education systems,
industry, agriculture and economies in general. The impact is magnified because
AIDS weakens and kills many young adults, people in their most productive years.
So many farmers and farmworkers have died of AIDS that the U.N. has invented the
term ''new variant famine.'' It means that because of AIDS, the continent will
experience persistent famine for generations instead of the usual cycles of
hunger tied to variable weather.
Africa's misery hangs like a sword over Asia, Eastern Europe and the Caribbean.
Researchers don't expect the infection rates to rival those in Africa. But
Asia's population is so big that even low infection rates could easily translate
into tens of millions of deaths.
Although fewer than 1 percent of its people are infected, India has topped South
Africa as the country with the most infections, 5.7 million to 5.5 million,
according to UNAIDS.
The astonishing numbers have grown from a humble beginning.
Nobody knows for sure when or where, but the AIDS epidemic is thought to have
begun in the primeval forests of West Africa when a virus lurking in the blood
of a monkey or a chimpanzee made the leap from one species to another, infecting
a hunter.
Researchers have found HIV in a blood sample collected in 1959 from a man in
Kinshasa, Congo. Genetic analysis of his blood suggested the HIV infection
stemmed from a single virus in the late 1940s or early 1950s.
For decades at least, the early human infections went unnoticed on a continent
where life routinely is harsh, short and cheap.
Then, on June 5, 1981, the Centers for Disease Control in Atlanta reported five
young actively homosexual men in Los Angeles had a new, mysterious and as yet
unnamed illness that attacked the immune system and caused a type of pneumonia.
A month later, it reported an odd surge among homosexual men in the number of
cases of Karposi Sarcoma, a rare cancer now linked to AIDS.
In the early days of the epidemic, just the mention of AIDS elicited snickers
and jokes. Few saw it as a major threat. It was the ''Gay Plague,'' and for
some, divine retribution for a lifestyle Christian fundamentalists and other
conservatives consider deviant and sinful.
When heterosexuals began to contract the disease through blood transfusions and
other medical procedures, they were often portrayed as ''innocent'' victims of a
disease spread by the immoral and licentious behavior of others.
The initial reactions and prejudices associated with AIDS slowed the early
response to the epidemic and limited the funding. Too much time, money and
effort was spent on the wrong priorities, Stirling aid.
''Over the last 25 years, the one real weakness was the search for the magic
bullet. There is no quick and simple fix,'' he said. ''But with the recent
successes we are starting to see the end of epidemic.''
''There is evidence to suggest we are at the tipping point,'' said Stirling.
The pace of change over the last couple of years suggests the number of new
infections can be reduced by 50 to 60 percent by 2020 -- if the momentum
continues.
''It is surely possible, it is doable,'' Stirling said.
AP correspondent Mike Stobbe in Atlanta
contributed to this report.
AIDS Toll May Reach
100 Million in Africa,
NYT,
4.6.2006,
http://www.nytimes.com/aponline/
world/AP-AIDS-at-25-Africa.html - broken link
Explore more on these topics
Anglonautes > Vocapedia
viruses >
retro-viruses > HIV
animals > apes, monkeys
AIDS/HIV activism
microbes > viruses
Coronaviruses, dengue, Ebola, Flu,
Hepatitis B and C,
HIV, Measles, mpox,
Polio, Smallpox,
Yellow fever, Zika
body,
health, medicine, drugs,
viruses, bacteria,
diseases / illnesses,
hygiene, sanitation,
health care / insurance
genetics
genetics > gene therapy, gene editing >
CRISPR
mental health, psychology
health,
contraception, abortion,
pregnancy, birth, life,
life expectancy,
getting older / aging,
death
USA > prescription opioid painkillers
lifestyle / health >
exercise,
smoking / tobacco, vaping,
drinking / alcohol,
diet, obesity
religions > Christians > popes
Related > Anglonautes > Arts > TV series
UK > It's a Sin
Related > Anglonautes > Arts > Drama
Larry Kramer
USA 1935-2020
Related > Anglonautes >
Arts
Robert Mapplethorpe USA 1946-1989
Freddie Mercury UK 1946-1991
|